Written by Steven Hansen
The U.S. new cases 7-day rolling average are 14.2 % LOWER than the 7-day rolling average one week ago. U.S. hospitalizations due to COVID-19 are now 10.5 % LOWER than the rolling average one week ago. U.S. deaths due to coronavirus are now 4.9 % HIGHER than the rolling average one week ago. Today’s posts include:
- U.S. Coronavirus New Cases are 166,113
- U.S. Coronavirus hospitalizations are at an elevated 101,003
- U.S. Coronavirus deaths are at an elevated 3,604
- U.S. Coronavirus immunizations have been administered to 8.4 % of the population
- The 7-day rolling average rate of growth of the pandemic shows new cases worsened, hospitalizations improved, and deaths improved
- Current charts are showing a “holiday” peak is behind us – hopefully, this improving trend will remain in play even with the new strains
- Fauci: Variants ‘Wake Up Call’ for COVID Vax Efforts
- Deadlier or not? The latest COVID-19 mutations and you
- Johnson & Johnson Executive Says Vaccine Works Where It Counts: Preventing Deaths
- Johnson & Johnson’s vaccine offers strong protection but fuels concern about variants
- There will be enough Covid vaccines for the ‘entire U.S. adult population by June,’ Johnson & Johnson board member says
- How the COVID Vaccines by J&J, Moderna, Pfizer, Astrazeneca Are Different
- Tough Pain Relief Choices in the COVID-19 Pandemic
- Clinicians Struggle to Make Sense of ‘Long COVID’
- CDC Mask Mandate: What to Know About Changes to Travel
- OSHA takes its first steps under Biden to tighten Covid-19 safety practices at work

The recent worsening of the trendlines for new cases is behind us which was attributed to going back to college/university, cooler weather causing more indoor activities, mutation of the virus, fatigue from wearing masks / social distancing, holiday activities, and some loosening of regulations designed to slow the coronavirus spread.
My continuing advice is to continue to wash your hands (especially after using the toilet as COVID first sheds in your stool), putting down the toilet seat (as flushing the toilet releases a plume), wear masks, avoid crowds, and maintain social distancing. No handwashing, mask, or social distancing will guarantee you do not get infected – but it sure as hell lowers the risk in all situations – and the evidence to-date shows a lower severity of COVID-19. In addition, certain activities are believed to carry a higher risk – like being inside in air conditioning and removing your mask (such as restaurants, around your children/grandchildren, bars, and gyms). It is all about viral load – and outdoor activities are generally safe if you can maintain social distance. Finally, studies show eating right (making sure you are supporting your immune system) and adequate sleep increase your ability to fight off COVID.
include($_SERVER[‘DOCUMENT_ROOT’].’/pages/coronavirus1.htm’); ?>
Hospitalizations (grey line) and Mortality (green line)
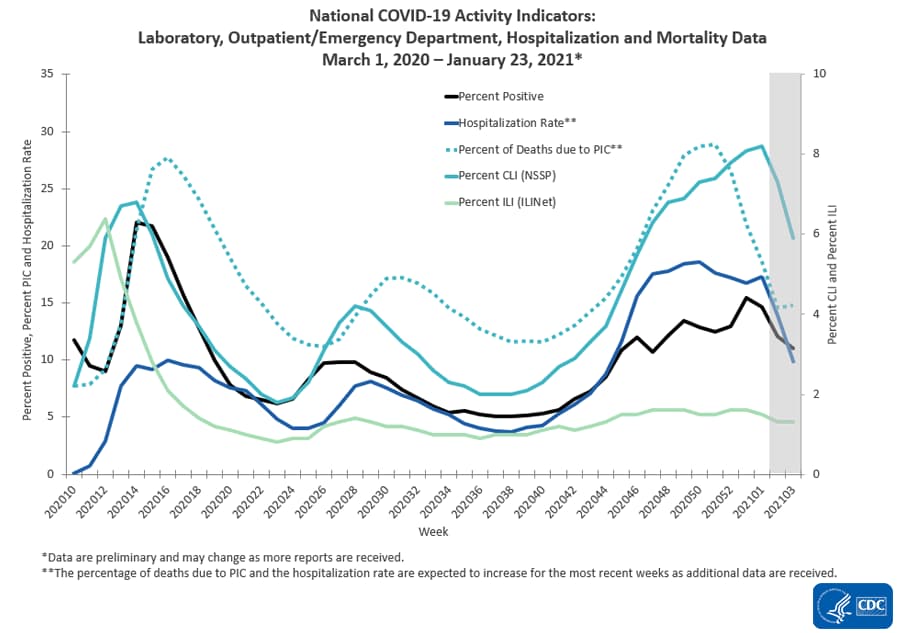
source: https://www.cdc.gov/coronavirus/2019-ncov/covid-data/covidview/index.html
Hospitalizations Are The Only Accurate Gauge As Reporting Is Not Affected By Holidays
The 4 day Thanksgiving holiday period put the first wobble in the trends. Over weekends and holidays, the number of new cases and deaths decline. Over weekends, this is not a problem for week-over-week rolling averages as weekends are compared against the previous weekend. But when a holiday falls within a working week, a non-working day is compared to a working day which causes havok in the trends.
However, hospitalizations historically appear to be little affected by weekends or holidays – the daily counts do not vary significantly from day-to-day.
The hospitalization growth rate trend is improving.

For the Thanksgiving and the end of the year holiday period – roughly, it seems each appears to have added around 5 % to the rate of growth of new cases, hospitalizations, and deaths.
Historically, hospitalization growth follows new case growth by one to two weeks.
As an analyst, I use the rate of growth to determine the trend. But, the size of the pandemic is growing in terms of real numbers – and if the rate of growth does not become negative – the pandemic will overwhelm all resources.
The graph below shows the rate of growth relative to the growth a week earlier updated through today [note that negative numbers mean the rolling averages are LOWER than the rolling averages one week ago]. As one can see, the rate of growth for new cases peaked in early December 2020 for Thanksgiving, and early January 2021 for end of year holidays – and the rate of growth is now contracting.

In the scheme of things, new cases decline first, followed by hospitalizations, and then deaths.
It is up to each of our readers to protect themselves and others by washing your hands, wearing a mask, avoiding crowds, and maintaining social distancing.
Will The New Variants Cause The Next Spike?
Maybe and maybe not. It all depends on vaccinations:
- the more people that are vaccinated reduces the pool of people that can be infected. Today we have removed over 7% of the population from being infected which theoretically should reduce the infection rate by 7% [it is unstudied whether the vaccines prevent a vaccinated person from being a carrier of the virus even though showing no signs]. If the vaccines are shown to stop transmission, then in theory it would reduce the infection rate by double the percent vaccinated [in this case you prevent your own infection and do not pass it along to another].
- it is also unknown what the effective rate of the current vaccines is against mutations that seem to appear almost daily. As an example, if the effective rate drops to 60%, it means the 7% reduction in the infection rate discussed above is almost cut in half. The South African and Brazilian variant is somewhat immune to the current vaccines.
- The pandemic should be over immediately if everyone could be vaccinated today. The problem is that every day brings a new mutation (which would not appear if the pandemic was stopped). The longer the immunization process takes – the more ineffective the vaccine will become.
- It is not clear whether the vaccine prevents those vaccinated from spreading the virus. It seems to be well documented that it normally stops the virus from taking hold and when it does not – the infection is mild.
Coronavirus News You May Have Missed
Fauci: Variants ‘Wake Up Call’ for COVID Vax Efforts – MedPage
SARS-CoV-2 variants from the U.K., South Africa, Brazil, and even the U.S. will require researchers to be “nimble” to keep up with them, and make vaccination against the virus even more essential, Anthony Fauci, MD, said at a White House COVID-19 press briefing on Friday.
Fauci, director of the National Institute for Allergy and Infectious Diseases, acknowledged that evidence from vaccine trials in South Africa demonstrate that these variants have real-world clinical impact.
Release of topline results Thursday afternoon from two trials of Novavax’s protein subunit vaccine, one of which was conducted in South Africa, was followed Friday morning by a similar announcement from Johnson & Johnson on its phase III trial, which included a South African cohort. Both showed significantly lower vaccine efficacy than in participants elsewhere, and genomic analysis indicated that a substantial fraction of the cases in South African vaccine recipients involved the novel variant.
Previously, Fauci had said he believed that current vaccines would remain clinically effective against the novel variants, but the Novavax and Johnson & Johnson data call that into question. Novavax, for example, reported efficacy of 60% in the South African cohort; in its British trial, efficacy was 95.6% against the original coronavirus strain and 85.6% against the so-called U.K. variant, also known as B.1.1.7.
“Even though … severe disease was still handled reasonably well by the vaccines, it is a wake-up call to all of us that we will continue to see the evolution of mutants,” Fauci said at the Friday briefing.
New coronavirus variant has caused reinfection in South Africa, Fauci says – CNN
Dr. Anthony Fauci, the top US infectious disease expert, says colleagues in South Africa have told him some patients there have been reinfected with the coronavirus due to the new, more contagious, variant.
“When we were communicating with our many scientific and public health colleagues in South Africa, they were telling us over the phone ‘something strange is going on right now, we have people who were infected several months ago, who now with this new strain are getting reinfected,'” Fauci told NBC News’ Lester Holt on Friday.
“Which is telling you that the immune response induced to the first infection wasn’t good enough to prevent the second infection.”However, Fauci said vaccination appears to be “good or better than natural infection in preventing further infection.”
“The vaccine itself appears to be better at inducing that kind of protection because they had anywhere from 50 to 88% efficacy against severe disease,” said Fauci, Director of the US National Institute of Allergy and Infectious Diseases.
[editor’s note: also read US now has more than 400 cases of coronavirus variant first identified in UK, CDC reports]
Clinicians Struggle to Make Sense of ‘Long COVID’ – MedPage
The only pattern in so-called “long COVID” is there is no pattern, as it appears to affect even those who experienced more mild disease, specialists told clinicians on a CDC call on Thursday.
“Long COVID” is nebulous, particularly because it can overlap with other complications of COVID-19 illness, such as hospitalization complications and post-intensive care syndrome, or even multisystem inflammatory disorder, said Alfonso Hernandez-Romieu, MD, of the CDC.
And there is no standardized definition of the condition, either. Persistent severe fatigue, headache, “brain fog,” and mild cognitive impairment are some of the most commonly presenting symptoms, and patients tend to present more than 4 weeks after illness. However, Hernandez-Romieu noted that these symptoms can be independent of disease severity, and can be newly occurring or recurring symptoms.
For example, Hernandez-Romieu said that research out of China showed that three-quarters of patients hospitalized with COVID-19 said they had at least one “ongoing” symptom, and one in five patients not requiring supplemental oxygen during hospitalization reported decreased lung function after 6 months.
While long COVID symptoms span a variety of specialties, respiratory and neurological complaints are among the most common. Jennifer Possick, MD, of Yale University School of Medicine in New Haven, Connecticut, discussed her experience with long COVID in a pulmonary specialty clinic. In her experience, dyspnea, fatigue, and exertional intolerance were most commonly reported, with patients reporting multiple symptoms simultaneously, and a quarter of patients reporting dyspnea 6 months post-infection.
… She described the “dominant pattern” of post-COVID pulmonary disease as patients with persistent symptoms with normal pulmonary function tests and thoracic imaging.
She shared her initial clinical model, which included imaging, pulmonary function tests, and 6-minute walk tests, and repeating selected labs to the initial diagnostics when a patient presented with symptoms. Though she noted patients with normal pulmonary function tests did not need repeat imaging, tests were generally repeated at 3, 6, and 12 months, as needed, for severity, along with extrapulmonary consultation.
… Allison Navis, MD, of Icahn School of Medicine at Mount Sinai in New York City, described her experiences with this type of program at her hospital. She also said most patients she was seeing had what would be considered “mild COVID,” with a broad range of symptoms, most of which would not be considered pure neurological syndromes with objective deficits.
“Brain fog,” she said, was the most common neurological symptom, which she described as a combination of issues with short-term memory, concentration, and word-finding or speech difficulty. There was no correlation with the severity of COVID, and the impact on patients varied, with symptoms fluctuating (“good and bad days”).
Other neurological symptoms that patients reported included headaches, which also followed no clear pattern of either migraines or tension headaches, as well as paresthesias, such as tingling or numbness, and dysautonomia, including light-headedness, palpitations, and gastrointestinal disturbances.
Johnson & Johnson Executive Says Vaccine Works Where It Counts: Preventing Deaths – NPR
Dr. Paul Stoffels, the chief scientific officer at Johnson & Johnson, told NPR on Friday that the topline results from the company’s coronavirus vaccine study fail to tell the full story about just how effective it actually is.
Johnson & Johnson said that 28 days after vaccination, its vaccine is 66% effective in preventing moderate to severe cases of COVID-19. But Stoffels says that Johnson & Johnson’s vaccine is very effective where it matters most: preventing hospitalizations and deaths.
“We showed that there was an 85% efficacy against severe disease and a complete protection against hospitalization and complete protection against death. And that’s across all the regions, including in South Africa,” he says.
A new coronavirus variant that was first discovered in South Africa has already popped up in the U.S. Johnson & Johnson’s vaccine was 57% effective in preventing moderate to severe cases in that country, where the variant dominates. But it was still 89% effective in stopping severe disease, hospitalization and death in South Africa, Stoffels says.
Johnson & Johnson’s study included participants in the U.S., Argentina, Brazil, Chile, Colombia, Mexico, Peru and South Africa. Unlike the two-dose vaccines by Pfizer and Moderna, Johnson & Johnson’s vaccine is administered as a single dose.
“That’s very remarkable results: that we can show with a single dose that we can prevent across the world, at 85%, all severe cases and complete[ly] for death and hospitalization,” Stoffels says.
- The United States has ordered 100 million doses of the Johnson & Johnson vaccine, which the company plans to deliver by June.
- “Assuming all of the close review of the J&J data all pans out, we’re going to have the capacity between Moderna, Pfizer, J&J, to have enough vaccines available by June for the entire U.S. adult population,” said McClellan.
- J&J’s vaccine was found to be 66% effective overall in preventing moderate to severe Covid.
Deadlier or not? The latest COVID-19 mutations and you – The Hill
Variants of the SARS-COV-2 virus caused by mutations are spreading widely and fear is spreading with them. Most of the public never heard of viral variants until recently and, for many, the news sounds like something out of a sci-fi movie.
The South Africa variant known as B.1.351 has now been found in South Carolina and there is concern that the new vaccines may not be fully effective against it. Pfizer has studied it and the good news is that, in the laboratory at least, there is still a significant degree of protection provided by their vaccine.
With the United Kingdom (U.K.) variant, the worry is different. Is it more virulent? Will you be more likely to die if you get it? The answer is that we really don’t know, since we lack the ability to trace it properly. Hospitalizations and deaths are easier to track than case numbers. Tracking variants needs genetic tests that are not performed routinely.
From the beginning of the pandemic in China, studies have shown that a large proportion of the mild infections have gone undocumented. This means that we vastly overestimated the death rate because we underestimated the number of cases.
This problem has persisted. Recent studies have shown that one in five to one in three people who are infected with the original SARS-COV-2 virus experience no symptoms whatsoever.
The SARS-COV-2 variant B.1.1.7 now predominating in the U.K., and spreading here in the U.S., appears to be much easier to transmit, with estimates as high as 50 to 70 percent more so. But a virus that spreads more easily can do so with a lower viral load, which leads to more asymptomatic cases and is even more difficult to detect. Our COVID-19 tests are less accurate when the viral load is lower and the symptoms are fewer. According to the Food and Drug Administration (FDA), there likely are far more false-negative results, or cases missed, with the new genetic variants. The more that cases are missed, the higher the death rate will appear to be.
According to data published by the U.K. government, the London School of Hygiene and Tropical Medicine reviewed 1.2 million people tested for COVID-19 and found that, among 2,583 deaths which occurred over a month, patients were 30 percent more likely to have the new variant. Sir Patrick Vallance, the government’s chief scientific adviser, said that, with the new variant, there was an increase of the death rate over the age of 60, from 10 to between 13 and 14 out of 1,000, but he acknowledged that only a small subset of cases were considered. For the vast majority of deaths, it was unclear which variant was involved. And patients reportedly were not dying of this strain once they were in the hospital — a sign that it really may not be more virulent.
If the virus is slightly more deadly now, it is likely due to the current winter weather.
Economist Richard Carson and a group of expert modeling researchers at University of California, San Diego, and the Massachusetts Institute of Technology (MIT) matched daily temperatures during the pandemic with death rates. They were able to determine that the virus became more virulent at lower temperatures and that around 40 degrees Fahrenheit was ideal for the virus. By the time the weather dropped to 5 degrees Celsius (41 degrees Fahrenheit), the model showed deaths rising by 160 percent due only to the influence of cold weather. This increase in cold weather was true regardless of genetic variant.
Tough Pain Relief Choices in the COVID-19 Pandemic – Medscape
More people with fever and body aches are turning to nonsteroidal anti-inflammatory drugs (NSAIDs) to ease symptoms, but the drugs have come under new scrutiny as investigators work to determine whether they are a safe way to relieve the pain of COVID-19 vaccination or symptoms of the disease.
Early on in the pandemic, French health officials warned that NSAIDs, such as ibuprofen, could worsen coronavirus disease, and they recommended switching to acetaminophen instead.
The National Health Service in the United Kingdom followed with a similar recommendation for acetaminophen.
But the European Medicines Agency took a different approach, reporting “no scientific evidence” that NSAIDs could worsen COVID-19. The US Food and Drug Administration also opted not to take a stance.
The debate prompted discussion on social media, with various reactions from around the world. It also inspired Craig Wilen, MD, PhD, from Yale University School of Medicine in New Haven, Connecticut, and his team to examine the effect of NSAIDs on COVID-19 infection and immune response. Their findings were published online January 20 in the Journal of Virology.
“It really bothered me that nonevidence-based decisions were driving the conversation,” Wilen said. “Millions of people are taking NSAIDs every day and clinical decisions about their care shouldn’t be made on a hypothesis.”
One theory is that NSAIDs alter susceptibility to infection by modifying angiotensin-converting enzyme 2 (ACE2). The drugs might also change the cell entry receptor for SARS-CoV-2, alter virus replication, or even modify the immune response.
CDC Mask Mandate: What to Know About Changes to Travel – Newsweek
The U.S. Centers for Disease Control and Prevention issued a sweeping mask mandate for Americans using transportation as part of the effort to stop the spread of COVID-19.
The 11-page order issued on Friday night will make it a federal offense not to wear masks on public and commercial transport. The mandate will take effect at 11:59 p.m. ET on Monday.
The order applies to trains, buses, planes, boats, ferries, subways and ride-hail vehicles. It will also take effect in transport hubs such as train stations, bus depots and airport terminals.
The mask mandate will not apply military vehicles, commercial trucks or children under two years of age.
Transportation workers and operators will also be required to wear masks. Travelers will be allowed to eat and drink briefly with their masks off.
“Requiring masks on our transportation systems will protect Americans and provide confidence that we can once again travel safely even during this pandemic,” said the order, which was signed by Marty Cetron, director for CDC‘s Division of Global Migration and Quarantine.
Those refusing to wear masks in compliance with the order could potentially face criminal charges but the CDC suggested it was more likely that violators would incur civil penalties, according to Reuters. The CDC also said they would largely rely on “widespread voluntary compliance.”
[editor’s note: From late Monday, all Americans will have to wear masks on public transport]
How the COVID Vaccines by J&J, Moderna, Pfizer, Astrazeneca Are Different – Newsweek
Johnson & Johnson
The Johnson & Johnson vaccine only requires one shot, which the company has said it will provide on a “non-profit” basis for the duration of the pandemic—costing around $10 a dose.
While an ongoing Phase III clinical trial assessing the vaccine has yet to be completed, the company has announced that the vaccine was 66 percent effective overall in preventing moderate to severe COVID-19, 28 days after vaccination, according to an interim analysis.
Notably, there were differences in efficacy results depending on the location. For example, the efficacy was 72 percent among trial volunteers in the U.S., but 66 percent in Latin America and 57 percent in South Africa—where a new more infectious variant has taken hold—at 28 days after vaccination.
But the vaccine candidate was 85 percent effective in preventing severe disease across all the regions that were studied.
The vaccine is based on a modified adenovirus—a common virus that causes cold-like symptoms—that has been engineered to carry pieces of genetic material from the “spike protein” of SARS-CoV-2, which causes COVID-19.
Pfizer-BioNTech
The Pfizer-BioNTech COVID-19 vaccine requires two doses, which should be administered 21 days apart.
The vaccine was authorized for emergency use by the FDA on December 11, 2020—becoming the first COVID-19 shot to receive regulatory approval in the U.S.
The vaccine, which is based on mRNA technology, has an efficacy of 95 percent. It contains tiny fragments of genetic code from the SARS-CoV-2 virus, which are injected into the body, enabling the immune system to build up defenses against the disease.
Moderna
The Moderna COVID-19 vaccine also requires two doses, which should be administered 28 days apart.
Like the Pfizer-BioNTech shot, the vaccine is based on mRNA technology. Clinical trials have shown it be around 95 percent effective.
AstraZeneca-University of Oxford
The vaccine developed by AstraZeneca-University of Oxford has been shown to have an overall efficacy of around 70 percent in large-scale clinical trials.
The vaccine was authorized for emergency use in the U.K. in December, and on Friday the European Medicines Agency approved the shot for use across the 27 member states of the European Union. It likely won’t receive approval in the U.S. until spring.
The vaccine, which is based on similar modified adenovirus technology to the Johnson & Johnson candidate, requires two doses administered 28 days apart.
Johnson & Johnson’s vaccine offers strong protection but fuels concern about variants. – New York Times
Johnson & Johnson said on Friday that its one-dose coronavirus vaccine provided strong protection against Covid-19, offering the United States a third powerful tool in a race against a worldwide rise in virus mutations.
But the results came with a significant cautionary note: The vaccine’s efficacy rate dropped from 72 percent in the United States to 57 percent in South Africa, where a highly contagious variant is driving most cases. Studies suggest that this variant also blunts the effectiveness of Covid vaccines made by Pfizer-BioNTech, Moderna and Novavax.
The variant has spread to at least 31 countries, including two cases documented in the United States this week.
Johnson & Johnson said it planned to apply for emergency authorization of its vaccine from the Food and Drug Administration as soon as next week, putting it on track to receive clearance later in February.
“This is the pandemic vaccine that can make a difference with a single dose,” said Dr. Paul Stoffels, the company’s chief scientific officer.
… Many researchers say it is imperative to vaccinate people as quickly as possible. Lowering the rate of infection could thwart the more contagious variants while they are still rare.
“If ever there was reason to vaccinate as many people as expeditiously as we possibly can with the vaccine that we have right now, now is the time,” said Dr. Anthony S. Fauci, the government’s top infectious disease expert. “Because the less people that get infected, the less chance you’re going to give this particular mutant a chance to become dominant.”
OSHA takes its first steps under Biden to tighten Covid-19 safety practices at work. – New York Times
The federal occupational safety agency on Friday posted new guidance for employers on reducing the spread of Covid-19 in the workplace, just over one week after President Biden signed an executive order directing it to do so.
The move by the Occupational Safety and Health Administration, part of the Labor Department, includes only recommendations, not requirements. But the agency said it was exploring a rule mandating certain protective measures.
The agency declined to issue such a rule, known as an emergency temporary standard, during the Trump administration. But Mr. Biden indicated support for a standard during the campaign.
The new guidance makes fewer distinctions than the Trump administration’s version based on the exposure risk of different workers. “Everyone should be protected, not some more protected than others,” Ann Rosenthal, a senior adviser to the agency, said on a video call with reporters.
The document issued on Friday also uses less equivocal language than the agency did under President Donald J. Trump. For example, it says the most effective prevention programs “ensure that absence policies are nonpunitive.” During the Trump administration, the agency advised employers to “ensure that sick leave policies are flexible and consistent with public health guidance.”
The following are foreign headlines with hyperlinks to the posts
Deaths After Pfizer COVID Vaccines Not Linked to Shots: EU Medicine Agency
The W.H.O. drops opposition to vaccinations for pregnant women
The Philippines tells kids to stay home and ‘glue their attention to TV.’
France and Germany, alarmed by variants, will restrict incoming travelers.
A fight between the EU and UK reveals the ugly truth about vaccine nationalism
Italy to ease virus restrictions in many regions from Sunday
EU will not trigger Brexit protocol amid vaccine export dispute, European Commission says
The following additional national and state headlines with hyperlinks to the posts
Navajo Nation Begins Mass Vaccinations After Lifting Lockdown Order
Fauci hopes to see vaccinations for children by ‘late spring and early summer’
Prolonged Liver Disease Can Follow Severe COVID-19
‘COVID Tongue’ May Be a Symptom, Professor Says
Top 10 Technology Hazards: Pandemic Plays Key Role
Rep. Stephen Lynch Tests Positive for COVID-19 Despite Full Vaccination
COVID-19 Becomes Leading Cause of Death in U.S. in January, Study Shows
‘It’s numbing’: Nine retired nuns in Michigan died of Covid-19.
Most states have opened vaccines to older Americans, according to a Times survey.
Moderna is said to have asked the FDA to allow it to put additional doses in its vaccine vials, a source familiar with the matter told CNBC. The move seeks to alleviate a bottleneck in Covid-19 vaccine manufacturing.
Biotech firm Novavax expects to produce up to 150 million Covid-19 vaccine doses per month by May or June, CEO Stanley Erck told Reuters.
United Airlines told 14,000 employees, some of whom were recently called back to work, that their jobs are at risk when a second round of federal payroll aid expires at the end of March.
Today’s Posts On Econintersect Showing Impact Of The Pandemic With Hyperlinks
January 2021 Chemical Activity Barometer Rises And Returns To Expansion
December 2020 Coincident Indices Generally Show Slowing Economic Conditions
COVID-19s Impact On U.S. Home Production
Warning to Readers
The amount of politically biased articles on the internet continues to increase. And studies and opinions of the experts continue to contradict other studies and expert opinions. Honestly, it is difficult to believe anything anymore. A study usually cannot establish cause and effect – but only correlation. Be very careful what you believe about this pandemic.

I assemble this coronavirus update daily – sifting through the posts on the internet. I try to avoid politically slanted posts (mostly from CNN, New York Times, and the Washington Post) and can usually find unslanted posts on that subject from other sources on the internet. I wait to publish posts on subjects that I cannot validate across several sources. But after all this extra work, I do not know if I have conveyed the REAL facts. It is my job to provide information so that you have the facts necessary – and then it is up to readers to draw conclusions.
Analyst Opinion of Coronavirus Data
There are several takeaways that need to be understood when viewing coronavirus statistical data:
- The global counts are suspect for a variety of reasons including political. Even the U.S. count has issues as it is possible that as much as half the population has had coronavirus and was asymptomatic. It would be a far better metric using a random sampling of the population weekly. In short, we do not understand the size of the error in the tracking numbers.
- Just because some of the methodology used in aggregating the data in the U.S. is flawed – as long as the flaw is uniformly applied – you establish a baseline. This is why it is dangerous to compare two countries as they likely use different methodologies to determine who has (and who died) from coronavirus.
- COVID-19 and the flu are different but can have similar symptoms. For sure, COVID-19 so far is much more deadly than the flu. [click here to compare symptoms]
- From an industrial engineering point of view, one can argue that it is best to flatten the curve only to the point that the health care system is barely able to cope. This solution only works if-and-only-if one can catch this coronavirus once and develops immunity. In the case of COVID-19, herd immunity may need to be in the 80% to 85% range. WHO warns that few have developed antibodies to COVID-19 when recovering from COVID-19. Herd immunity does not look like an option without immunization although there is now a discussion of whether T-Cells play a part in immunity [which means one might have immunity without antibodies]
- Older population countries will have a significantly higher death rate as there is relatively few hospitalizations and deaths in younger age groups..
- There are at least 8 strains of the coronavirus. New York may have a deadlier strain imported from Europe, compared to less deadly viruses elsewhere in the United States.
- Each publication uses different cutoff times for its coronavirus statistics. Our data uses 11:00 am London time. Also, there is an unexplained variation in the total numbers both globally and in the U.S.
What we do or do not know about the coronavirus [actually there is little scientifically proven information]. Most of our knowledge is anecdotal, from studies with limited subjects, or from studies without peer review.
- How many people have been infected as many do not show symptoms?
- Masks do work. Unfortunately, early in the pandemic, many health experts — in the U.S. and around the world — decided that the public could not be trusted to hear the truth about masks. Instead, the experts spread a misleading message, discouraging the use of masks.
- Current thinking is that we develop 5 months of immunity from further COVID infection.
- The Moderna and Pfizer vaccines have an effectiveness rate of about 95 percent after two doses. That is on par with the vaccines for chickenpox and measles. The 95 percent number understates the effectivenessas it counts anyone who came down with a mild case of Covid-19 as a failure. But turning Covid into a typical flu — as the vaccines evidently did for most of the remaining 5 percent — is actually a success. Of the 32,000 people who received the Moderna or Pfizer vaccine in a research trial, only one contracted a severe Covid case.
- To what degree do people who never develop symptoms contribute to transmission? Research early in the pandemic suggested that the rate of asymptomatic infections could be as high as 81%. But a meta-analysis, which included 13 studies involving 21,708 people, calculated the rate of asymptomatic presentation to be 17%.
- The accuracy of rapid testing is questioned – and the more accurate test results are not being given in a timely manner.
- Can children widely spread coronavirus? [current thinking is that they are a minor source of the pandemic spread]
- Why have some places avoided big coronavirus outbreaks – and others hit hard?
- Air conditioning contributes to the pandemic spread.
- It appears that there is increased risk of infection and mortality for those living in larger occupancy households.
- Male patients have almost three times the odds of requiring intensive treatment unit (ITU) admission compared to females.
- Outdoor activities seem to be a lower risk than indoor activities.
- Will other medical treatments for Covid-19 ease symptoms and reduce deaths? So far only remdesivir, Bamlanivimab,
and Regeneron) are approved for treatment. What drugs work?
Arthritis drugs tocilizumab and sarilumab could cut relative risk of death of those in intensive care by 24%
- A current scientific understanding of the way the coronavirus works can be found [here].
There is now a vaccine available – the questions remain:
- how effective it will be in the general population,
- will there be any permanent side effects that will appear months from now,
- how long immunity will last [we can currently say we do not know if it will last more than 4 months],
- there is no evidence the vaccine will block transmission
Heavy breakouts of coronavirus have hit farmworkers. Farmworkers are essential to the food supply. They cannot shelter at home. Consider:
- they have high rates of respiratory disease [occupational hazard]
- they travel on crowded buses chartered by their employers
- few have health insurance
- they cannot social distance and live two to four to a room – and they eat together
- some reports say half are undocumented
- they are low paid and cannot afford not to work – so they will go to work sick
- they do not have access to sanitation when working
- a coronavirus outbreak among farmworkers can potentially shutter entire farm
The bottom line is that COVID-19 so far has been shown to be much more deadly than the data on the flu. Using CDC data, the flu has a mortality rate between 0.06 % and 0.11 % Vs. the coronavirus which to date has a mortality rate of 4 % [the 4% is the average of overall statistics – however in the last few months it has been hovering around 1.0%] – which makes it between 10 and 80 times more deadly. The reason for ranges:
Because influenza surveillance does not capture all cases of flu that occur in the U.S., CDC provides these estimated ranges to better reflect the larger burden of influenza.
There will be a commission set up after this pandemic ends to find fault [it is easy to find fault when a once-in-a-lifetime event occurs] and to produce recommendations for the next time a pandemic happens. Those that hate President Trump will conclude the virus is his fault.
Resources:
- Get the latest public health information from CDC: https://www.coronavirus.gov .
- Get the latest research from NIH: https://www.nih.gov/coronavirus.
- Find NCBI SARS-CoV-2 literature, sequence, and clinical content: https://www.ncbi.nlm.nih.gov/sars-cov-2/.
- List of studies: https://icite.od.nih.gov/covid19/search/#search:searchId=5ee124ed70bb967c49672dad
include(“/home/aleta/public_html/files/ad_openx.htm”); ?>







