Written by Steven Hansen
The U.S. new cases 7-day rolling average is 6.4 % HIGHER than the 7-day rolling average one week ago. U.S. deaths due to coronavirus are now 3.4 % HIGHER than the rolling average one week ago. At the end of this post is a set of interactive graphs and tables for the world and individual States – as well as today’s headlines which include;
- Global new coronavirus cases again at record levels
- The Tree That Could Help Stop the Pandemic
- Tocilizumab, an immune modulator for rheumatoid arthritis, saves lives if given to critically ill COVID-19 patients within the first two days of being admitted to an ICU
- Glaring Gap Between Vit D Guidance and Practice in Care Homes
- Studies Point To Big Drop In COVID-19 Death Rates
- ICUs Without Air Conditioning Could Shield Doctors From COVID-19: Study
- Lilly hires external adviser for COVID-19 drug plant problems
- Except in areas where Covid is surging, there are still no lines of patients in the hospital halls
- How the F.D.A. Stood Up to the President
- First COVID-19 Wave Offers ICUs Lessons for Next Time
- More than 7 in 10 Gen-Zers report symptoms of depression during pandemic, survey finds
- With stimulus stalled, shortfalls in tax revenues leave states facing layoffs, service cuts

The recent worsening of the trendlines for new cases should be attributed to going back to college/university, cooler weather causing more indoor activities, and continued loosening of regulations designed to slow the coronavirus spread.
My continuing advice is to continue to wash your hands, wear masks, and maintain social distancing. No handwashing, mask, or social distancing will guarantee you do not get infected – but it sure as hell lowers the risk in all situations – as the evidence to-date shows a lower severity of COVID-19. In addition, certain activities are believed to carry a higher risk – like being inside in air conditioning and removing your mask (such as restaurants, around your children/grandchildren, bars, and gyms). It is all about viral load – and outdoor activities are generally safe.
The daily number of new cases in the U.S. is remaining stubbornly and embarrassedly high – and is currently increasing.
The following graphs show the 7-day rolling average for new coronavirus cases and deaths have been updated through 21 October 2020:


z coronavirus.png
Hospitalizations (grey line) and Mortality (green line) For Week ending 10OCT2020
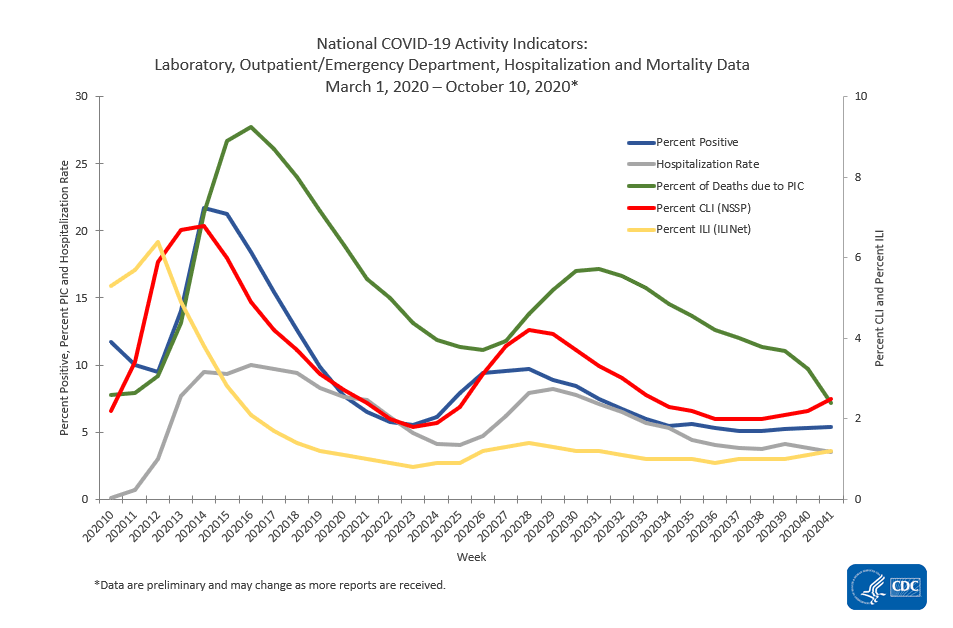
source: https://www.cdc.gov/coronavirus/2019-ncov/covid-data/covidview/index.html
Coronavirus Statistics For 21 October 2020 |
| U.S. Only | Global | U.S Percentage of Total | ||||
| Today*** | Cumulative | Today*** | Cumulative | Today | Cumulative | |
| New Confirmed Cases | 59,512 | 8,270,000 | 372,207 | 40,860,000 | 16.0% | 20.2% |
| Deaths** | 933 | 221,066 | 6,209 | 1,130,000 | 15.0% | 19.6% |
| Mortality Rate | 1.6% | 2.7% | 1.7% | 2.8% | ||
total COVID-19 Tests per 1,000 people | 1.91* | 407.12* | ||||
Source: EU CDC – The data insignificantly varies from the data produced by Johns Hopkins
* as of 17 Oct 2020
** evidently several States included “probable” deaths today in the number
*** red color indicates record number
Coronavirus News You May Have Missed
More than 7 in 10 Gen-Zers report symptoms of depression during pandemic, survey finds – CNBC
From increased stress and anxiety to rising levels of loneliness, the mental health consequences of the Covid-19 pandemic are wide-sweeping. A new survey from the American Psychological Association points to the age group that’s been hit hardest: Gen-Z.
Gen-Z adults, those ages 18 to 23, reported the highest levels of stress compared to other generations and were the most likely age group to report symptoms of depression, according to the APA’s 2020 Stress in America survey.
More than seven in 10 Gen-Z adults surveyed said they experienced common symptoms of depression in the prior two weeks, such as: feeling so tired they sat around and did nothing, having trouble thinking and concentrating and feeling very restless, lonely, miserable or unhappy.
So why is Gen-Z hit so hard with stress and depression during the pandemic? They are “experiencing adulthood at a time when the future looks uncertain,” while older generations might have more perspective that enables them to cope with the changes, according to the report.
Fear and anxiety tend to run hand-in-hand, Kevin Antshel, clinical psychologist and director of the clinical psychology program at Syracuse University previously told CNBC Make It. “The more things are uncertain, the more we’re going to fear, and the more we fear things, the more we are anxious,” he said. And prolonged anxiety can lead to depression.
ICUs Without Air Conditioning Could Shield Doctors From COVID-19: Study – Medscape
Intensive care units (ICUs) at hospitals treating COVID-19 patients should do away with air-conditioning to limit the risk of infecting doctors, a study from a top Indian research institute has said.
Frontline health workers around the world have borne the brunt of the coronavirus crisis. More than 500 doctors have died from COVID-19 in India – the world’s second-worst hit nation – as infections near 8 million, straining the country’s weak and underfunded public health system.
“The recirculation of the air by the centralized air-conditioning systems is what has led to the significant infection of our committed medical fraternity and has also led to deaths of doctors and nurses,” the study by the Indian Institute of Science in Bengaluru, considered one of the country’s best science universities, said.
Reducing recirculation of air and increasing the use of outdoor air can lower the risk of spreading coronavirus in indoor spaces, the World Health Organisation has said.
Previous studies have suggested countries in hot climates should take care that indoor rooms are not dried out by overcooling with air conditioning, noting that keeping indoor humidity levels between 40% and 60% will help limit airborne transmission of the virus.
Studies Point To Big Drop In COVID-19 Death Rates – NPR
Two new peer-reviewed studies are showing a sharp drop in mortality among hospitalized COVID-19 patients. The drop is seen in all groups, including older patients and those with underlying conditions, suggesting that physicians are getting better at helping patients survive their illness.
“We find that the death rate has gone down substantially,” says Leora Horwitz, a doctor who studies population health at New York University’s Grossman School of Medicine and an author on one of the studies, which looked at thousands of patients from March to August.
The study, which was of a single health system, finds that mortality has dropped among hospitalized patients by 18 percentage points since the pandemic began. Patients in the study had a 25.6% chance of dying at the start of the pandemic; they now have a 7.6% chance.
That’s a big improvement, but 7.6% is still a high risk compared with other diseases, and Horwitz and other researchers caution that COVID-19 remains dangerous.
The death rate “is still higher than many infectious diseases, including the flu,” Horwitz says. And those who recover can suffer complications for months or even longer. “It still has the potential to be very harmful in terms of long-term consequences for many people.”
How the F.D.A. Stood Up to the President – New York Times
… despite the White House refusal to approve the new vaccine guidance document, the F.D.A. published the guidelines in briefing materials to an advisory committee that will discuss them on Thursday, effectively making them official. And nearly two weeks after Mr. Trump called the antibody treatment he received when sick with Covid-19 a miraculous “cure” and said that he had authorized it, the F.D.A. has not yet approved it.
Internally, Dr. Hahn has tried to erect a shield between his staff and White House officials, asking that all calls be routed directly to him and not to his staff. His situation is especially fraught because Mr. Trump has openly accused the F.D.A. of engaging in political ploys to harm his re-election chances. Alex M. Azar II, the secretary of health and human services and Dr. Hahn’s direct superior, has also questioned Dr. Hahn’s motives in some conversations with the White House, according to multiple officials.
A senior administration official, who spoke on condition of anonymity, denied that Dr. Hahn and Mr. Meadows were deeply at odds over the vaccine guidance, saying “the two have a good relationship.” Mr. Meadows’s only concern was that changing the guidance in the middle of ongoing clinical trials could confuse vaccine makers, said the official, who noted that the White House eventually approved it.
[editor’s note: this article has sections in it which are politically biased]
Lilly hires external adviser for COVID-19 drug plant problems – Reuters
Eli Lilly and Co LLY.N said late on Tuesday it had hired an independent consultant to review a plant producing its COVID-19 antibody drug after receiving a notice from the U.S. health regulator.
The company reiterated that it had not received a warning letter from the U.S. Food and Drugs Administration (FDA) following its plant inspection, which was first reported by Reuters last week.
It received an Official Action Indicated (OAI) notice from the FDA in relation to issues at its Branchburg plant in New Jersey, Lilly reiterated. (bit.ly/3m9z1AE)
Reuters on Oct. 13 reported that inspectors who visited Lilly’s plant in Branchburg, New Jersey last November found data on various manufacturing processes had been deleted and not appropriately audited, according to government inspection documents.
Following its November inspection, the FDA classified the problems as the most serious level of violation, resulting in an OAI notice.
The problems could complicate the drugmaker’s bid for an emergency use authorization from the federal agency for its COVID-19 drug.
Human coronaviruses ‘inactivated’ by mouthwash, oral rinses – Fox News
A new study conducted by researchers at the Penn State College of Medicine has found that a common dental item can inactivate human coronaviruses: mouthwash and oral rinses
For the study, the results of which were published in the Journal of Medical Virology, researchers tested various oral and nasopharyngeal rinses — which included a 1% solution of baby shampoo, a neti pot, peroxide sore-mouth cleansers, and mouthwashes — to determine how well they inactivated human coronaviruses.
The baby shampoo solution, “which is often used by head and neck doctors to rinse the sinuses,” the researchers noted in a news release regarding the findings, was particularly effective; the solution inactivated “greater than 99.9% of human coronavirus after a two-minute contact time,” they said.
The mouthwash and oral rinses were also efficacious, they found: “Many inactivated greater than 99.9% of virus after only 30 seconds of contact time and some inactivated 99.99% of the virus after 30 seconds.”
More specifically, researchers “used a test to replicate the interaction of the virus in the nasal and oral cavities with the rinses and mouthwashes,” as the nasal and oral cavities are thought to be main points of entry for human coronaviruses, including SARS-CoV-2, better known as COVID-19. Though the researchers didn’t specifically test SARS-CoV-2 in the study, the novel virus is genetically similar to the other human coronaviruses tested, leading the researchers to hypothesize that the results would be similar.
A strain of human coronavirus was mixed with “baby shampoo solutions, various peroxide antiseptic rinses and various brands of mouthwash,” allowing the solutions to interact with the virus for different amounts of time, including 30 seconds, one minute, and two minutes. The solutions were then diluted to “prevent further virus inactivation,” they wrote.
… Lead study author Craig Meyers, a distinguished professor of microbiology and immunology and obstetrics and gynecology, said the results show that the amount of virus (viral load) in an infected person’s mouth could be reduced by using these common over-the-counter products, ultimately helping to reduce the spread of the novel virus.
Where Have All the Hospital Patients Gone? Except in areas where Covid is surging, there are still no lines of patients in the hospital halls. – New York Times
In pre-pandemic times, patients … were routine at my Boston-area hospital; we saw them almost every day. But for much of the spring and summer, the halls and parking lots were eerily empty. I wondered if people were staying home and getting sicker, and I imagined that in a few months’ time these patients, once they became too ill to manage on their own, might flood the emergency rooms, wards and I.C.U.s, in a non-Covid wave.
But more than seven months into the pandemic, there are still no lines of patients in the halls. While my colleagues and I are busier than we were in March, there has been no pent-up overflow of people with crushing chest pain, debilitating shortness of breath or fevers and wet, rattling coughs.
… Researchers from Sound Physicians, a national medical group of almost 4,000 doctors specializing in hospital medicine, critical care and emergency medicine, and the Dartmouth Institute for Health Policy and Clinical Practice gathered admissions data from more than 200 hospitals in 36 states and compared differences in patient characteristics, diagnoses and mortality rates between February and July of this year with the same time period last year. The researchers found that by mid-April, non-Covid admissions to hospitals had dropped by almost half.
… But surprisingly, even months later, as coronavirus infection rates began falling and hospitals were again offering elective surgery and in-person visits to doctor’s offices, hospital admissions remained almost 20 percent lower than normal.
First COVID-19 Wave Offers ICUs Lessons for Next Time – MedPage
The first wave of COVID-19 forced hospitals to get creative when treating patients, and they can apply these lessons as the next wave of the pandemic approaches.
“This is teaching us that no one is immune and no one is going to be omitted from this,” said David Ferraro, MD, of National Jewish Health in Denver, during a presentation at the virtual CHEST conference, the annual meeting of the American College of Chest Physicians.
“We all have to … learn how to surge and stock supplies. Be prepared to have a plan A, a plan B, and a plan C,” Ferraro said.
Innovative solutions, such as using alternative drugs from another drug class; using an equivalent within the drug class family; or changing the route of administration can help to alleviate medication shortages, which are an ongoing public health crisis, even pre-COVID-19, he said. The pandemic only upended an already vulnerable supply chain, battling lack of incentives to produce less profitable drugs, and a market that had difficulty responding to disruptions.
Because medication production surges do not occur quickly, and the FDA previously acknowledging the potential for drug shortages, this becomes a problem in an ongoing public health crisis, with over 50,000 COVID-19 cases per day in the U.S., Ferraro said.
In particular, sedatives, analgesics, and paralytic agents are among those agents at risk of shortages. Ferraro said, specifically citing propofol, fentanyl, dexmedetomidine, and midazolam among the medications in short supply.
[editor’s note: if this subject interests you, this article deserves a full read]
The list of drugs shown effective for treating COVID-19 got longer Tuesday, even as another well-used drug lost some of its luster.
In a large clinical study, tocilizumab, an immune modulator long used to treat rheumatoid arthritis, showed it can save lives if given to critically ill COVID-19 patients within the first two days of being admitted to an intensive care unit.
The study, published in JAMA Internal Medicine, showed just over 27% of ICU patients treated with tocilizumab died within a month, compared with 37% of those just as seriously ill but did not receive the drug.
Tocilizumab, a so-called monoclonal antibody, has been used during the outbreak because of its effect on tamping down immune over-reactions, which have been common with COVID-19. Smaller studies, including one published at the same time by the same journal have shown mixed results, with some finding the drug did not reduce deaths.
With stimulus stalled, shortfalls in tax revenues leave states facing layoffs, service cuts – USA Today
A combination of COVID-19 and plunging oil prices have caused states’ tax revenues to drop more than 6% during the six months from the first pandemic shutdowns in March through the end of August.
The 46 states that have reported their tax figures for the period show a combined revenue drop of nearly $30 billion compared with the same stretch last year, according to the Urban Institute, a Washington, D.C. think tank that analyzes tax policy and other issues.
Oil and gas producing states were the first to feel the impact as plummeting worldwide demand and prices in February rocked their economies only to be quickly followed by COVID-19 retail closures in March and April. The lack of sales activity meant dramatically lower tax collections at least for the first few months of the crisis.
Glaring Gap Between Vit D Guidance and Practice in Care Homes – Medscape
Vitamin D supplementation in elderly care home residents is largely viewed as a “medicine” rather than a protective nutrient, risking vitamin D deficiency in this particularly vulnerable population, say British public health scientists.
Writing in BMJ Nutrition Prevention & Health, they stress an urgent review is needed of the nutritional guidelines and regulations in England on the use of the vitamin in elderly residential care homes.
Vitamin D supplementation “needs a professional separation from medicine and reframing as a matter of public health nutrition as well as a medical responsibility,” emphasizes Joe Williams, MSc Public Health graduate, Brighton University, UK, and colleagues.
The findings reveal “both a failure to implement evidence-based recommendations and a social injustice in urgent need of public health advocacy and resolution,” they emphasize.
For 30 years, vitamin D 10 µg as a daily supplement has been endorsed for care home residents. In 2016, the recommendations were extended to the entire population in the winter months and throughout the year for those living in care homes.
But this new study shows care home staff understood that they were only allowed to give residents vitamin supplements that have been prescribed and that physicians had been advised by the UK National Health Service not to prescribe preventative vitamins because they can be bought cheaply over the counter.
… Vitamin D deficiency increases not only the risk of bone fractures, but could also make people more susceptible to SARS-CoV-2 infection and worsen outcomes.
U.S. Coronavirus Cases Will Rapidly Rise in the Next Week, Says Expert
A leading health expert expects new coronavirus infections to increase rapidly across the country over the next week, while also predicting that deaths from COVID-19 will jump in the coming weeks.
New COVID-19 infections are growing higher or remain elevated in 31 states, according to the New York Times tracker. Meanwhile, new cases remain low in just seven states—Delaware, Maryland, California, New York, Hawaii, Maine and Vermont. Nationwide, the U.S. reported 60,598 new infections and 929 deaths from COVID-19 on Tuesday, bringing the totals for the pandemic to more than 8.3 million cases and nearly 221,000 deaths.
“If you look at states, you know, particularly throughout the midwest and plains, we’re seeing record cases almost everyday,” Dr. Jonathan Reiner, a professor of Medicine at the George Washington University Medical Center, told CNN on Wednesday morning. Reiner pointed out that the seven-day average of new cases is now about 60,000 per day. “But it’s on the rise. Soon it will be 70,000 cases,” he said.
5 factors that could make you more at risk of suffering from ‘long Covid’ – CNBC
A new study has identified the main factors that make it more likely that coronavirus patients will suffer long term effects from the virus.
“Long Covid” is the term given to people who recover from coronavirus but continue to suffer from a wide range of symptoms, such as shortness of breath, migraines and chronic fatigue.
A new analysis by researchers at King’s College London, using data from the COVID Symptom Study app, shows that 1 in 20 people with Covid-19 are likely to suffer symptoms for at least eight weeks.
The team found that older or overweight people, women, those with asthma and those with a greater number of different symptoms in the first week of their illness were more likely to develop “long Covid.”
The Tree That Could Help Stop the Pandemic – The Atlantic
… Erck is the CEO of Novavax, a Maryland-based maker of vaccines. Not a seller of vaccines, mind you: The company had yet to bring one of its candidates to market. But like other companies around the world, Novavax had thrown its hat into the coronavirus-vaccine race. And its success, Erck believed, depended on that odd ingredient in Slurpees.
The inner bark of the Chilean soapbark tree, Quillaja saponaria, is the source material for some of these saponins. Pulverized and soaked in water at the Desert King factory in Chile, the bark is transformed into a brown, bitter, bubbly fluid. This precious goo does many things well, and it happens to be the raw material for one of the world’s most coveted vaccine adjuvants: QS-21. Adjuvants are compounds that boost the body’s immune reaction to a vaccine. Owing to their potential risks to human health, however, only a handful of adjuvants have been approved by the U.S. Food and Drug Administration, and QS-21 is one of the newest.
A single gram of powdered QS-21 costs more than $100,000, though only about $5 worth is needed for each shot. Nine years ago, researchers estimated that the global supply of pharmaceutical-grade Quillaja extract was sufficient for just 6 million doses of vaccine. Everyone in the business knew the story of the Pacific yew tree, whose bark was the original source of the chemotherapy drug paclitaxel, and which was threatened by large-scale harvesting in the 1980s. “If you take out all the trees in one shot and deplete the source of saponin, you are in deep shit in the future,” says Garo Armen, whose company, Agenus, helped bring QS-21 to market. Novavax has its own saponin-based adjuvant, called Matrix-M, and warned investors last year that their vaccines could be delayed if they failed to “secure sufficient supplies” of high-quality extract. And the Hileys practically had a monopoly on it.
During his call with the Hileys, Erck asked if Desert King could increase their production for Novavax a hundredfold. Paul Hiley’s jaw dropped to the table. Novavax was on the cusp of receiving $384 million in international funding to help it produce 100 million doses of its COVID-19 vaccine for the world by the end of the year, and a billion doses by the end of 2021. It would also soon be on the short list of vaccine candidates funded by the Trump administration’s Operation Warp Speed. Novavax needed guarantees of 1,500 pounds of saponin now, and up to three times as much next year.
Hiley’s immediate concern was that his Chilean operation had already missed the bark-harvesting window—typically during the trees’ spring growth, between September and December. And last year he had made the ill-timed decision to postpone expanding their pharmaceutical operations in favor of investing in Desert King’s booming animal-feed business.
In the end, Hiley knew there was only one way to answer Erck: “Of course, we can deliver it,” he said. Three months later, inside the Desert King conference room in early July, sitting across from a shelf displaying Slurpee cups and bottles of Stewart’s Root Beer, Hiley let out a chuckle through his surgical mask. “I had no idea if we could.”
The following are foreign headlines with hyperlinks to the posts
Ireland To Impose 6-Week National Lockdown, Estimates 150,000 Job Losses
Sweden’s COVID Strategist Wants to Ease Restrictions for Elderly
Scientists raise doubts about Britain’s plan to deliberately infect volunteers.
Thailand welcomes its first foreign tourists in months.
The Czech Republic will close shops and further tighten rules to stem its outbreak.
At a quarantine hotel in Australia, blood testing devices may have exposed some guests.
Brazilian volunteer in Oxford AstraZeneca coronavirus vaccine trial dies
German Health Minister Jens Spahn tests positive for coronavirus
Greece records its highest case increase since pandemic began
Western Cape [South Africa] sees 42% increase in COVID-19 cases
Czech Deputy Prime Minister Hamacek tests positive for COVID-19
The following are additional national and state headlines with hyperlinks to the posts
A woman in her 30s died from COVID-19 while on a plane from New Mexico to Texas.
AstraZeneca may resume its U.S. trial of a coronavirus vaccine as early as this week.
How dissecting superspreading events can help people take COVID-19 measures seriously
And how about getting them to take a vaccine? Learning about vaccine efficacy, adverse effects, and duration of protection will persuade them, researchers found.
U. Of Michigan Students Under Stay-In-Place Order, But Football Can Still Kick Off
NIH Director ‘Guardedly Optimistic’ About COVID-19 Vaccine Approval By End Of 2020
Pelosi bullish on COVID-19 deal: ‘Help is on the way’
DC cancels 2021 Cherry Blossom Parade over COVID-19 fears
Disney slams California officials for ‘unworkable’ guidelines around theme park reopening
Start Pediatric Vaccine Trials for COVID-19 Now, Experts Urge
Swing-State Voters Blame Trump, Pelosi Nearly Equally for Stimulus Failure
2 World Champion Swimmers Among 10 Others Who Test Positive for COVID-19
A court rules that a California prison ravaged by the virus must transfer inmates to protect them.
Conservatives press Trump to modernize the C.D.C.’s health data system.
White House says aid to states and cities is the biggest stimulus sticking point.
Worried about the virus in the winter? Alaska offers a cautionary tale.
Boston public schools suspend in-person reopening, citing a rise in the city’s positivity rate.
Federal Reserve Governor Lael Brainard said Congress needs to support more stimulus to address a recovery that so far has left out large parts of the U.S. economy
Today’s Posts On Econintersect Showing Impact Of The Pandemic With Hyperlinks
September 2020 Sea Container Imports Continue At Record Pace, Exports Not So Much
October 2020 Beige Book: Slight To Modest Growth Seen
Disneyland Fights Back After California Unveils Strict Reopening Rules
As Working From Home Continues, Video Interviewing Is Here To Stay
Fiscal Policy For An Unprecedented Crisis
Warning to Readers
The amount of politically biased articles on the internet continues to increase. And studies and opinions of the experts continue to contradict other studies and expert opinions. Honestly, it is difficult to believe anything anymore. A study usually cannot establish cause and effect – but only correlation. Be very careful what you believe about this pandemic.

I assemble this coronavirus update daily – sifting through the posts on the internet. I try to avoid politically slanted posts (mostly from CNN, New York Times, and the Washington Post) and can usually find unslanted posts on that subject from other sources on the internet. I wait to publish posts on subjects that I cannot validate across several sources. But after all this extra work, I do not know if I have conveyed the REAL facts. It is my job to provide information so that you have the facts necessary – and then it is up to readers to draw conclusions.
Coronavirus INTERACTIVE Charts
include($_SERVER[‘DOCUMENT_ROOT’].’/pages/coronavirus.htm’); ?>
Analyst Opinion of Coronavirus Data
There are several takeaways that need to be understood when viewing coronavirus statistical data:
- The global counts are suspect for a variety of reasons including political. Even the U.S. count has issues as it is possible that as much as half the population has had coronavirus and was asymptomatic. It would be a far better metric using a random sampling of the population weekly. In short, we do not understand the size of the error in the tracking numbers.
- Just because some of the methodology used in aggregating the data in the U.S. is flawed – as long as the flaw is uniformly applied – you establish a baseline. This is why it is dangerous to compare two countries as they likely use different methodologies to determine who has (and who died) from coronavirus.
- COVID-19 and the flu are different but can have similar symptoms. For sure, COVID-19 so far is much more deadly than the flu. [click here to compare symptoms]
- From an industrial engineering point of view, one can argue that it is best to flatten the curve only to the point that the health care system is barely able to cope. This solution only works if-and-only-if one can catch this coronavirus once and develops immunity. In the case of COVID-19, herd immunity may need to be in the 80% to 85% range. WHO warns that few have developed antibodies to COVID-19. At this point, herd immunity does not look like an option although there is now a discussion of whether T-Cells play a part in immunity [which means one might have immunity without antibodies]
- Older population countries will have a higher death rate.
- There are at least 8 strains of the coronavirus. New York may have a deadlier strain imported from Europe, compared to less deadly viruses elsewhere in the United States.
- Each publication uses different cutoff times for its coronavirus statistics. Our data uses 11:00 am London time. Also, there is an unexplained variation in the total numbers both globally and in the U.S.
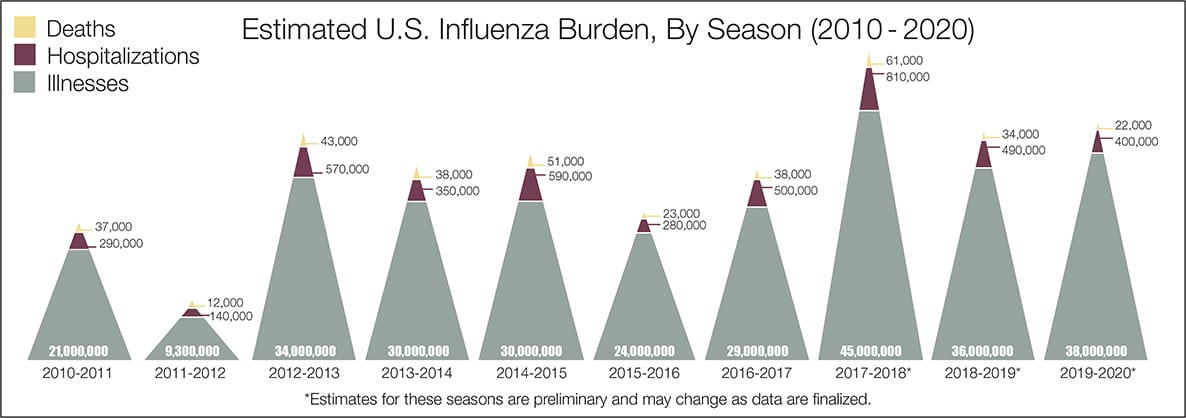
- The real question remains if the U.S. is over-reacting to this virus. The following graphic from the CDC puts the annual flu burden in perspective [click on image to enlarge]. Note that using this data is dangerous as the actual flu cases are estimated and not counted – nobody knows how accurate these guesses are.
What we do not know about the coronavirus [actually there is little scientifically proven information]. Most of our knowledge is anecdotal, from studies with limited subjects, or from studies without peer review.
- How many people have been infected as many do not show symptoms?
- Masks do work.
- Do we develop lasting immunity to the coronavirus? Another coronavirus – the simple cold – does not develop long term immunity.
- To what degree do people who never develop symptoms contribute to transmission?
- The US has scaled up coronavirus testing – and the accuracy of the tests has been improving. However, if one loses immunity – the coronavirus testing value is reduced.
- Can children widely spread coronavirus? [current thinking is that they are becoming a major source of the pandemic spread]
- Why have some places avoided big coronavirus outbreaks – and others hit hard?
- What effect will the weather have? At this point, it does not seem hot weather slows this coronavirus down – and it seems air conditioning contributes to its spread.
- Outdoor activities seem to be a lower risk than indoor activities.
- Can the world really push out an effective vaccine in 12 to 18 months?
- Will other medical treatments for Covid-19 ease symptoms and reduce deaths? So far only one drug (remdesivir) is approved for treatment.
- A current scientific understanding of the way the coronavirus works can be found [here].
Heavy breakouts of coronavirus have hit farm workers. Farmworkers are essential to the food supply. They cannot shelter at home. Consider:
- they have high rates of the respiratory disease [occupational hazard]
- they travel on crowded buses chartered by their employers
- few have health insurance
- they cannot social distance and live two to four to a room – and they eat together
- some reports say half are undocumented
- they are low paid and cannot afford not to work – so they will go to work sick
- they do not have access to sanitation when working
- a coronavirus outbreak among farmworkers can potentially shutter entire farm
The bottom line is that COVID-19 so far has been shown to be much more deadly than the data on the flu. Using CDC data, the flu has a mortality rate between 0.06 % and 0.11 % Vs. the coronavirus which to date has a mortality rate of 4 % [the 4% is the average of overall statistics – however in the last few months it has been hovering around 1.0%] – which makes it between 10 and 80 times more deadly. The reason for ranges:
Because influenza surveillance does not capture all cases of flu that occur in the U.S., CDC provides these estimated ranges to better reflect the larger burden of influenza.
There will be a commission set up after this pandemic ends to find fault [it is easy to find fault when a once-in-a-lifetime event occurs] and to produce recommendations for the next time a pandemic happens. Those that hate President Trump will conclude the virus is his fault.
Resources:
- Get the latest public health information from CDC: https://www.coronavirus.gov .
- Get the latest research from NIH: https://www.nih.gov/coronavirus.
- Find NCBI SARS-CoV-2 literature, sequence, and clinical content: https://www.ncbi.nlm.nih.gov/sars-cov-2/.
- List of studies: https://icite.od.nih.gov/covid19/search/#search:searchId=5ee124ed70bb967c49672dad
Human coronaviruses ‘inactivated’ by mouthwash, oral rinses
include(“/home/aleta/public_html/files/ad_openx.htm”); ?>