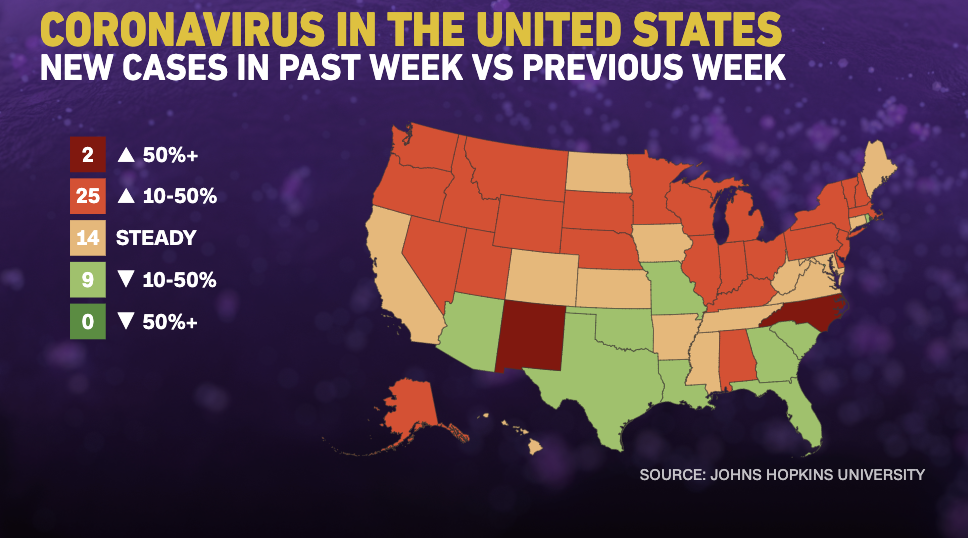
Written by Steven Hansen
The U.S. new cases 7-day rolling average is 5.2 % HIGHER than the 7-day rolling average one week ago. U.S. deaths due to coronavirus are now 1.8 % LOWER than the rolling average one week ago. At the end of this post is a set of interactive graphs and tables for the world and individual States – as well as today’s headlines which include;
- Loss of smell is highly reliable indicator of Covid-19 infection
- Does the common cold protect you from COVID?
- 61% of U.S. households with children report facing serious financial problems during the coronavirus outbreak
- Moderna says its coronavirus vaccine won’t be ready until 2021
- FDA broadens probe into serious illness in AstraZeneca coronavirus vaccine but the EU Is fast tracking
- Mosquitoes Don’t Help Spread Coronavirus
- Patients With Psych Disorders at Elevated Risk of COVID-19 Death

The recent worsening of the trendlines for new cases should be attributed to going back to school – especially at college/university level.
My continuing advice is to continue to wash your hands, wear masks, and maintain social distancing. No handwashing, mask, or social distancing will guarantee you do not get infected – but it sure as hell lowers the risk in all situations – and evidence to-date shows a lower severity of COVID-19. In addition, certain activities are believed to carry higher risk – like being inside in air conditioning and removing your mask (such as restaurants, around your children/grandchildren, bars, and gyms). It is all about viral load – and outdoor activities are generally very safe.
The daily number of new cases in the U.S. is remaining stubbornly and embarrassedly high.
The following graphs show the 7-day rolling average for new coronavirus cases and deaths have been updated through 01 October 2020:


z coronavirus.png
Coronavirus Statistics For 01 October 2020 |
| U.S. Only | Global | U.S Percentage of Total | ||||
| Today*** | Cumulative | Today*** | Cumulative | Today | Cumulative | |
| New Confirmed Cases | 42,691 | 7,230,000 | 292,026 | 34,030,000 | 14.6% | 21.2% |
| Deaths** | 930 | 206,928 | 5,934 | 1,020,000 | 15.7% | 20.3% |
| Mortality Rate | 2.2% | 2.9% | 2.0% | 3.0% | ||
total COVID-19 Tests per 1,000 people | 1.67* | 342.18* | ||||
* as of 26 Sep 2020
** evidently several States included “probable” deaths today in the number
*** red color indicates record number
Coronavirus News You May Have Missed
According to a new NPR/Robert Wood Johnson Foundation/Harvard T.H. Chan School of Public Health poll, 61% of U.S. households with children report facing serious financial problems during the coronavirus outbreak. Serious problems are reported across a wide range of areas during this time, including depleting household savings, serious problems paying credit card bills and other debt, and affording medical care (see Table 1).
Many of these problems are concentrated among Black and Latino households with children, households with children that have annual incomes below $100,000, and households with children that have experienced job or wage losses since the start of the outbreak. Serious financial problems are reported by large majorities of Latino (86%) and Black (66%) households with children, as well as about half (51%) of white households with children. In addition, about three in four (74%) households with children that have annual incomes below $100,000 report facing serious financial problems during the coronavirus outbreak.
When it comes to employment problems, 60% of households with children report any adult household members have lost their jobs, been furloughed, or had wages or hours reduced since the start of the outbreak. And among these households with job or wage losses during the coronavirus outbreak, about three in four (76%) report facing serious financial problems.
This poll, The Impact of Coronavirus on Households with Children, was conducted July 1 – August 3, 2020, among 3,454 U.S. adults ages 18 or older, including 1,000 adults in households who are living with children under age 18. Adults in this survey were asked to report on serious problems facing both themselves and others living in their households, so measures are reported as a percentage of households for all household-related questions.
Moderna says its coronavirus vaccine won’t be ready until 2021 – Axios
Moderna CEO Stéphane Bancel said Wednesday that his company’s coronavirus vaccine won’t be available for widespread distribution until at least spring 2021, according to Financial Times.
Why it matters: Bancel told FT that the drugmaker will not seek emergency authorization for FDA approval for its vaccine for front-line medical workers and at-risk individuals until Nov. 25 at the earliest.
- He added the company would not seek FDA approval for use in the general population until late January.
- If the vaccine is proven safe and effective, approval is unlikely to come until at least late March or early April.
What he’s saying: “I think a late [first quarter], early [second quarter] approval is a reasonable timeline, based on what we know from our vaccine,” Bancel said, according to FT.
The big picture: Moderna’s vaccine is one of four that are currently in late-stage testing in people in the U.S.
FDA broadens probe into serious illness in AstraZeneca coronavirus vaccine study – The Hill
The Food and Drug Administration (FDA) has reportedly broadened its investigation into a serious illness suffered by a patient participating in AstraZeneca’s COVID-19 vaccine testing trials.
Reuters reported Thursday that FDA officials will seek data from Oxford University, AstraZeneca’s testing partner, regarding trials of vaccines for other diseases unrelated to COVID-19 in the hopes of determining whether patients in those trials developed similar side effects.
The move comes after the AstraZeneca-Oxford project was put on hold in early September due to one British trial participant falling ill with what was believed to be the rare spinal condition transverse myelitis.
“It just shows that the FDA is being thorough,” one source familiar with the probe said to Reuters.
The widened scope of the probe reportedly does not indicate a view by the FDA that AstraZeneca’s trials are unsafe or that other vaccines used in trials by Oxford were unsafe either, according to the sources, who noted that some delays have occurred due to Oxford’s data being presented in a different format from what the FDA has requested.
[editor’s note: AstraZeneca’s Covid-19 Vaccine Put On Fast Track By EU Regulator]
Patients With Psych Disorders at Elevated Risk of COVID-19 Death – MedPage
Patients with mental illness are more at risk for severe COVID-19 outcomes than the general population, according to a study from a large hospital system.
Among 1,685 patients hospitalized with COVID-19, those with a prior psychiatric diagnosis had a significantly higher risk of death compared with patients without a diagnosis after controlling for demographic characteristics, comorbidities, and hospital location (HR 1.5, 95% CI 1.1-1.9, P=0.003), reported Luming Li, MD, of the Yale University School of Medicine in New Haven, Connecticut.
The risk was higher among patients with a psychiatric diagnosis at 2 weeks after their index hospitalization (35.7% vs 14.7%), as well as at 3 weeks (40.9% vs 22.2%) and 4 weeks (44.8% vs 31.5%), the team wrote in a research letter published in JAMA Network Open.
“Psychiatric symptoms may arise as a marker of systemic pathophysiologic processes, such as inflammation, that may, in turn, predispose to mortality,” the researchers wrote. “Similarly, psychiatric disorders may augment systemic inflammation and compromise the function of the immune system, while psychotropic medications may also be associated with mortality risk.”
This Overlooked Variable Is the Key to the Pandemic – The Atlantic
… There are COVID-19 incidents in which a single person likely infected 80 percent or more of the people in the room in just a few hours. But, at other times, COVID-19 can be surprisingly much less contagious. Overdispersion and super-spreading of this virus are found in research across the globe. A growing number of studies estimate that a majority of infected people may not infect a single other person. A recent paper found that in Hong Kong, which had extensive testing and contact tracing, about 19 percent of cases were responsible for 80 percent of transmission, while 69 percent of cases did not infect another person. This finding is not rare: Multiple studies from the beginning have suggested that as few as 10 to 20 percent of infected people may be responsible for as much as 80 to 90 percent of transmission, and that many people barely transmit it.
… This kind of behavior, alternating between being super infectious and fairly noninfectious, is exactly what k captures, and what focusing solely on R hides. Samuel Scarpino, an assistant professor of epidemiology and complex systems at Northeastern, told me that this has been a huge challenge, especially for health authorities in Western societies, where the pandemic playbook was geared toward the flu—and not without reason, because pandemic flu is a genuine threat. However, influenza does not have the same level of clustering behavior.
We can think of disease patterns as leaning deterministic or stochastic: In the former, an outbreak’s distribution is more linear and predictable; in the latter, randomness plays a much larger role and predictions are hard, if not impossible, to make. In deterministic trajectories, we expect what happened yesterday to give us a good sense of what to expect tomorrow. Stochastic phenomena, however, don’t operate like that—the same inputs don’t always produce the same outputs, and things can tip over quickly from one state to the other. As Scarpino told me, “Diseases like the flu are pretty nearly deterministic and R0 (while flawed) paints about the right picture (nearly impossible to stop until there’s a vaccine).” That’s not necessarily the case with super-spreading diseases.
[editor’s note: this post deserves a full read]
Big contact tracing study shows role of kids and superspreaders in coronavirus pandemic – CNN
Children can spread coronavirus among themselves efficiently, but young adults are the primary source of coronavirus spread, according to a study published Wednesday.
The study, based on a giant contact tracing effort involving more than 3 million people in India, shows most Covid-19 patients never infected anyone else. The researchers found that 70% of infected people did not infect any of their contacts, while 8% of patients accounted for 60% of observed new infections.
The study also contradicts the widely held belief that children are unlikely to catch the coronavirus.
“We find otherwise. They are getting infected in significant numbers,” study leader Ramanan Laxminarayan of the Center for Disease Dynamics, Economics and Policy in New Delhi, and also of Princeton University, told CNN.
… “We were surprised to find that just 8% of the infected primary cases were responsible for 60% of the contacts that were infected,” he said. “That’s a hugely disproportionate effect. Superspreading has been suspected, but not really documented.” Most of the index cases — the first patient in a chain of transmission — were adults aged 20 to 45, the team found.
“The young to middle adult age group is the one that is coming into contact with people. They are the people most likely to be outside the household. They are the ones taking the disease from one place to the other,” Laxminarayan said.
Coronavirus: does the common cold protect you from COVID? – The Conversation
… Scientists at La Jolla Institute for Immunology in California showed that infection with common cold coronaviruses can generate an immune response that resembles key pieces of the immune response generated by SARS-CoV-2 – the virus that causes COVID-19. This raises the possibility that previous infection with one of the milder coronaviruses could make COVID-19 less severe. But how likely is this? And how does this relate to what we already know about coronaviruses?
A few weeks ago, a different article sat at the centre of the SARS-CoV-2 immunity debate. This one showed that the antibody response to SARS-CoV-2 may decline over time.
The findings raised concern that SARS-CoV-2 could infect a person many times and that a vaccine might not generate lasting protection. But the article focused on just one arm of the immune response, the B cells, which produce antibodies that help to clear an infection.
T cells are also key to the immune response against viruses. They play a variety of roles, among them helping B cells to mature into disease-fighting machines. The article by Jose Mateus and colleagues at La Jolla Institute for Immunology is important because it shows that people keep T cells from the milder coronaviruses long enough to potentially interact with a new challenge by SARS-CoV-2 and that those T cells might even recognise SARS-CoV-2 and help to clear the infection.
… Evidence for cross-protection between all but the most closely related coronaviruses is scant.
It is difficult to say whether the milder coronaviruses protect against SARS-CoV-2 partly because we have done so little surveillance on them. Ideally, we would be able to look at historical data to identify which communities experienced major outbreaks of each milder coronavirus strain over the past few years and then see if there is a link with less severe COVID-19 cases.
White House Blocked C.D.C. Order to Keep Cruise Ships Docked – New York Times
The White House has blocked a new order from the Centers for Disease Control and Prevention to keep cruise ships docked until mid-February, a step that would have displeased the politically powerful tourism industry in the crucial swing state of Florida.
The current “no sail” policy, which was originally put in place in April and later extended, is set to expire on Wednesday. Dr. Robert R. Redfield, the director of the C.D.C., had recommended the extension, worried that cruise ships could become viral hot spots, as they did at the beginning of the pandemic.
But at a meeting of the coronavirus task force on Tuesday, Dr. Redfield’s plan was overruled, according to a senior federal health official who was not authorized to comment and so spoke on condition of anonymity. The administration will instead allow the ships to sail after Oct. 31, the date the industry had already agreed to in its own, voluntary plan, the agency announced late Wednesday night. The rejection of the C.D.C.’s original plan was first reported by Axios.
[editor’s note: this is a typical politically biased post by the New York Times. The economy is in danger of a double dip, and the tourism sector needs to be restarted. What I would expect of the CDC is to produce a strict set of guidelines to minimize the potential of COVID spread – and not a blanket approval of the mitigation efforts proposed by the cruise line industry. All activities outside the home carry varying elevated risks.]
NIH to assess and expand COVID-19 testing for underserved communities – NIH
The National Institutes of Health has awarded nearly $234 million to improve COVID-19 testing for underserved and vulnerable populations. A part of the Rapid Acceleration of Diagnostics (RADx) initiative, the RADx Underserved Populations (RADx-UP) program will support 32 institutions across the United States and will focus on populations disproportionately affected by the pandemic. These groups include African Americans, American Indians/Alaskan Natives, Latinos/Latinas, Native Hawaiians, older adults, pregnant women and those who are homeless or incarcerated.
“It is critical that all Americans have access to rapid, accurate diagnostics for COVID-19, especially underserved and vulnerable populations who are bearing the brunt of this disease,” said NIH Director Francis S. Collins, M.D., Ph.D. “The RADx-UP program will help us better understand and alleviate the barriers to testing for those most vulnerable and reduce the burden of this disease.”
The program aims to understand COVID-19 testing patterns better among underserved and vulnerable populations; strengthen the data on disparities in infection rates, disease progression and outcomes; and develop strategies to reduce these disparities in COVID-19 testing. To accomplish these goals in rapid fashion, the RADx-UP program is supporting projects with established community partnerships that can use their existing research infrastructures to swiftly implement strategies and interventions to increase access and uptake of COVID-19 testing among underserved and vulnerable populations.
The FDA and the Importance of Trust – The New England Journal of Medicine
As SARS-CoV-2 emerged, the global scientific community first studied the virus at the bench, then took what was learned to the bedside in the hope of helping patients, and later returned to the bench with observations from the bedside.1 Such a process has led to progress in the treatment and prevention of every important disease we have faced, including AIDS, cancer, and diabetes. In the case of SARS-CoV-2, the information we have gathered has increased our understanding of the biology of the virus, the diagnosis of the infection, the nature of the injury it causes, and potential therapies to treat it, but much is still unknown. In Covid-19, clinicians at the bedside continue to face an imperfectly understood disease that leads to tragic consequences for too many patients. Under enormous pressure to help patients while doing no harm, clinicians rely on the transparency of the scientific process and on the careful judgment of regulators who base their decisions on the best available scientific understanding of the disease.
Adequately sized and well-conducted randomized clinical trials are the foundation of evidence-based medicine, but they take time. As clinicians wait for trial data to emerge, they must often try available treatments without proof of their efficacy. This clinical urgency should not, however, be confused with knowledge of which treatment works and which has little value or may be harmful. Unbiased, transparent decisions by regulators are essential in times of uncertainty. Regulators ensure the essential steps of analyzing information from scientists and providing thoughtful guidance to clinicians and patients.
In the United States, the Food and Drug Administration (FDA) has the critical role of assessing emerging evidence to determine whether new therapies are safe and effective. Some of us serve or have served on FDA advisory committees and have first-hand knowledge of the FDA’s exhaustive, unbiased, highly informative review process. To minimize the possibility of bias, members of advisory committees and FDA panels must be free of relevant intellectual and financial conflicts of interest, and the FDA has historically operated with complete independence from other parts of the government, including the executive branch, from which it derives its authority.
… Determining the safety and efficacy of the therapies clinicians use and patients receive is at the heart of the medical system. The FDA has been the envy of the world, setting standards for the studies it requires and then following the resulting science and data in its regulatory decisions. Today more than ever, as science is being manipulated and disregarded, it is critical that the FDA uphold its standards and its objectivity. Truth may be difficult to know, but the scientific process is our best path to knowing it. Treatments for patients should evolve as new data accumulate. But physicians and patients must be confident that any approval from the FDA is based on a careful evaluation of all the available data and that the agency’s decisions are well reasoned and objective. There should be no political interference in the FDA process. The FDA and the executive branch should not squander the trust that the agency has carefully built over many decades of hard work.
United And American Airlines Tell 32,000 Employees They’re Now On Furlough – NPR
United Airlines and American Airlines have sent furlough notices to a total of more than 32,000 employees, saying they can’t afford to have them on payroll after Thursday – the expiration date for the federal CARES Act Payroll Support Program.
“To our departing 13,000 family members: thank you for your dedication and we look forward to welcoming you back,” United said in a message sent to employees Wednesday night that it also shared with NPR.
American sent a similar message to 19,000 employees, with CEO Doug Parker saying the furloughs could be reversed if Washington manages to reach a new business aid package. He also said there is hope for a CARES Act extension — and he pledged to immediately reverse the furloughs if a deal is reached “over the next few days.”
“I spoke late today with the Secretary of the Treasury Steven Mnuchin,” Parker said in a letter sent to employees on Wednesday. “He informed me that the White House and Speaker Nancy Pelosi are continuing to negotiate on a bipartisan COVID-19 relief package that would include an extension of the PSP and it is possible they could reach an agreement in the coming days.”
Mosquitoes Don’t Help Spread Coronavirus – MedPage
Mosquitoes and other biting insects can’t spread SARS-CoV-2, researchers reported, even if the blood suckers have had plenty of opportunity over the summer with everyone spending more time outside.
Unlike dengue, malaria, and Zika virus, the virus behind COVID-19 couldn’t replicate after being ingested by mosquitoes, Dana Mitzel, PhD, of the U.S. Department of Agriculture in Manhattan, Kansas, and colleagues reported on the preprint server bioRxiv without peer review.
Loss of smell is highly reliable indicator of Covid-19 infection – Evening Express
The findings suggest an acute loss of smell or taste is a highly reliable virus indicator, scientists say.
They add that loss of smell or taste should now be considered globally as a criterion for self-isolation, testing and contact tracing.
Researchers at UCL and UCLH (University College London Hospitals NHS Foundation Trust) assessed health data from primary care centres in London.
They found that 78% of people who reported sudden loss of smell and/or taste at the height of the pandemic had Covid-19 antibodies.
Of these people, 40% did not have a cough or fever.
According to the researchers it is the first time such a figure has been calculated.
The following are foreign headlines with hyperlinks to the posts
Sweden records highest daily rise in COVID-19 cases since June
Mexico has lost or discarded 5 percent of COVID-19 tests
Madrid Heads for Lockdown After Spain Announces New Virus Restrictions
Record Dutch COVID-19 Cases Prompt U-Turn on Face Masks
Italy reports 2,500 new cases in a day for the first time since April
World’s poorest countries receive $150 million to prepare for delivery of COVID-19 vaccines
Peru To Resume International Flights This Month
In new record, Israel records nearly 9,000 new cases
The following are additional national and state headlines with hyperlinks to the posts
Hospitals in Wisconsin have been forced to waitlist or transfer patients to other facilities as COVID-19 cases surge.
President Trump has yet to cancel campaign rallies scheduled in Wisconsin this weekend.
The pandemic has worsened food insecurity in Puerto Rico, as nearly half of the island stands to lose nutrition assistance and unemployment rates skyrocket.
Tennessee Titans Game Postponed Indefinitely After More Coronavirus Cases Reported
Study shows hydroxychloroquine did not prevent coronavirus in health care workers
North Dakota Saw 80 Percent Increase in COVID Cases in September
Entire Mississippi Middle School Forced to Quarantine
Pelosi and Mnuchin to talk again to try to break stimulus negotiation stalemate.
Fauci says public health measures to curb coronavirus spread could dampen flu season
H&M to close 250 shops as Covid drives sales online
US oil refiner Marathon Petroleum cuts 12% of staff because of pandemic
Today’s Posts On Econintersect Showing Impact Of The Pandemic With Hyperlinks
September 2020 ISM and Markit Manufacturing Surveys Little Changed
August 2020 Construction Spending Marginally Improves
August 2020 Real Personal Income Declined, Real Expenditures Improved
26 September 2020 Initial Unemployment Claims Rolling Average Again Declined

September 2020 Job Cuts: Year-to-Date Cuts At Record High
Warning to Readers
The amount of politically biased articles on the internet continues to increase. And studies and opinions of the experts continue to contradict other studies and expert opinions. Honestly, it is difficult to believe anything anymore. A study usually cannot establish cause and effect – but only correlation. Be very careful what you believe about this pandemic.

I assemble this coronavirus update daily – sifting through the posts on the internet. I try to avoid politically slanted posts (mostly from CNN, New York Times, and the Washington Post) and can usually find unslanted posts on that subject from other sources on the internet. I wait to publish posts on subjects that I cannot validate across several sources. But after all this extra work, I do not know if I have conveyed the REAL facts. It is my job to provide information so that you have the facts necessary – and then it is up to readers to draw conclusions.
Coronavirus INTERACTIVE Charts
include($_SERVER[‘DOCUMENT_ROOT’].’/pages/coronavirus.htm’); ?>
Analyst Opinion of Coronavirus Data
There are several takeaways that need to be understood when viewing coronavirus statistical data:
- The global counts are suspect for a variety of reasons including political. Even the U.S. count has issues as it is possible that as much as half the population has had coronavirus and was asymptomatic. It would be a far better metric using a random sampling of the population weekly. In short, we do not understand the size of the error in the tracking numbers.
- Just because some of the methodology used in aggregating the data in the U.S. is flawed – as long as the flaw is uniformly applied – you establish a baseline. This is why it is dangerous to compare two countries as they likely use different methodologies to determine who has (and who died) from coronavirus.
- COVID-19 and the flu are different but can have similar symptoms. For sure, COVID-19 so far is much more deadly than the flu. [click here to compare symptoms]
- From an industrial engineering point of view, one can argue that it is best to flatten the curve only to the point that the health care system is barely able to cope. This solution only works if-and-only-if one can catch this coronavirus once and develops immunity. In the case of COVID-19, herd immunity may need to be in the 80% to 85% range. WHO warns that few have developed antibodies to COVID-19. At this point, herd immunity does not look like an option although there is now a discussion of whether T-Cells play a part in immunity [which means one might have immunity without antibodies]
- Older population countries will have a higher death rate.
- There are at least 8 strains of the coronavirus. New York may have a deadlier strain imported from Europe, compared to less deadly viruses elsewhere in the United States.
- Each publication uses different cutoff times for its coronavirus statistics. Our data uses 11:00 am London time. Also, there is an unexplained variation in the total numbers both globally and in the U.S.
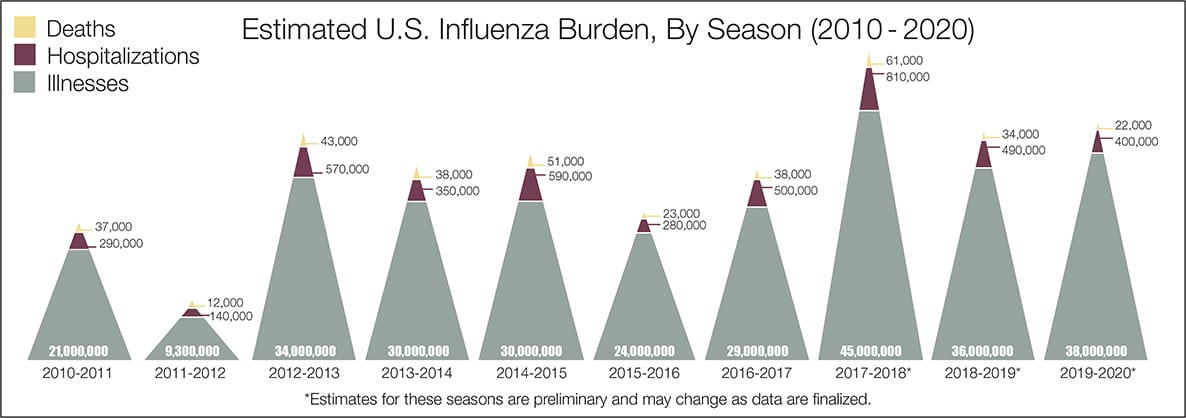
- The real question remains if the U.S. is over-reacting to this virus. The following graphic from the CDC puts the annual flu burden in perspective [click on image to enlarge]. Note that using this data is dangerous as the actual flu cases are estimated and not counted – nobody knows how accurate these guesses are.
What we do not know about the coronavirus [actually there is little scientifically proven information]. Most of our knowledge is anecdotal, from studies with limited subjects, or from studies without peer review.
- How many people have been infected as many do not show symptoms?
- Masks do work.
- Do we develop lasting immunity to the coronavirus? Another coronavirus – the simple cold – does not develop long term immunity.
- To what degree do people who never develop symptoms contribute to transmission?
- The US has scaled up coronavirus testing – and the accuracy of the tests has been improving. However, if one loses immunity – the coronavirus testing value is reduced.
- Can children widely spread coronavirus? [current thinking is that they are becoming a major source of the pandemic spread]
- Why have some places avoided big coronavirus outbreaks – and others hit hard?
- What effect will the weather have? At this point, it does not seem hot weather slows this coronavirus down – and it seems air conditioning contributes to its spread.
- Outdoor activities seem to be a lower risk than indoor activities.
- Can the world really push out an effective vaccine in 12 to 18 months?
- Will other medical treatments for Covid-19 ease symptoms and reduce deaths? So far only one drug (remdesivir) is approved for treatment.
- A current scientific understanding of the way the coronavirus works can be found [here].
Heavy breakouts of coronavirus have hit farm workers. Farmworkers are essential to the food supply. They cannot shelter at home. Consider:
- they have high rates of the respiratory disease [occupational hazard]
- they travel on crowded buses chartered by their employers
- few have health insurance
- they cannot social distance and live two to four to a room – and they eat together
- some reports say half are undocumented
- they are low paid and cannot afford not to work – so they will go to work sick
- they do not have access to sanitation when working
- a coronavirus outbreak among farmworkers can potentially shutter entire farm
The bottom line is that COVID-19 so far has been shown to be much more deadly than the data on the flu. Using CDC data, the flu has a mortality rate between 0.06 % and 0.11 % Vs. the coronavirus which to date has a mortality rate of 4 % [the 4% is the average of overall statistics – however in the last few months it has been hovering around 1.0%] – which makes it between 10 and 80 times more deadly. The reason for ranges:
Because influenza surveillance does not capture all cases of flu that occur in the U.S., CDC provides these estimated ranges to better reflect the larger burden of influenza.
There will be a commission set up after this pandemic ends to find fault [it is easy to find fault when a once-in-a-lifetime event occurs] and to produce recommendations for the next time a pandemic happens. Those that hate President Trump will conclude the virus is his fault.
Resources:
- Get the latest public health information from CDC: https://www.coronavirus.gov .
- Get the latest research from NIH: https://www.nih.gov/coronavirus.
- Find NCBI SARS-CoV-2 literature, sequence, and clinical content: https://www.ncbi.nlm.nih.gov/sars-cov-2/.
- List of studies: https://icite.od.nih.gov/covid19/search/#search:searchId=5ee124ed70bb967c49672dad
include(“/home/aleta/public_html/files/ad_openx.htm”); ?>