Written by Steven Hansen
The U.S. new cases 7-day rolling average is 8.9 % lower than the 7-day rolling average one week ago. U.S. deaths due to coronavirus are now 16.4 % lower than the rolling average one week ago. At the end of this post is a set of interactive graphs and tables for the world and individual States – as well as today’s headlines which include;
- Infectious COVID-19 Can Persist in Gut for Weeks
- Study links coronavirus mortality to air pollution exposure
- CDC says Covid-19 death rate is under 1% for everyone but people over 70
- Colleges are now hot spots, as nursing homes and meatpacking plants were earlier in the pandemic
- Persistent Lung Damage Improves Gradually After COVID-19
- The most dangerous phase of the US Covid-19 crisis may be yet to come
- Which Hospital Workers Face Least COVID Risk?
- What Happened To The Instant Hospitals Built For COVID-19 Patients In Wuhan?
- Italy is calling back coronavirus survivors in Bergamo. About half say they haven’t fully recovered.

My continuing advice is to continue to wash your hands, wear masks, and maintain social distancing. No handwashing, mask, or social distancing will guarantee you do not get infected – but it sure as hell lowers the risk in all situations – and evidence to-date shows a lower severity of COVID-19. In addition, certain activities are believed to carry higher risk – like being inside in air conditioning and removing your mask (such as restaurants, around your children/grandchildren, bars, and gyms). It is all about viral load – and outdoor activities are generally very safe.
The daily number of new cases in the U.S. is remaining stubbornly and embarrassedly high.
The following graphs show the 7-day rolling average for new coronavirus cases and deaths have been updated through 11 September 2020:


z coronavirus.png
Coronavirus Statistics For 11 September 2020 |
| U.S. Only | Global | U.S Percentage of Total | ||||
| Today*** | Cumulative | Today*** | Cumulative | Today | Cumulative | |
| New Confirmed Cases | 35,224 | 6,400,000 | 264,351 | 28,200,000 | 13.3% | 22.7% |
| Deaths** | 974 | 191,789 | 6,000 | 910,078 | 16.2% | 21.1% |
| Mortality Rate | 2.8% | 3.0% | 2.3% | 3.2% | ||
total COVID-19 Tests per 1,000 people | 1.39* | 286.20* | ||||
* as of 08 Sep 2020
** evidently several States included “probable” deaths today in the number
*** red color indicates record number
Coronavirus News You May Have Missed
The coronavirus may have reached Los Angeles even before China announced its outbreak – LA Times
Was the novel coronavirus on the loose in Los Angeles way back in December, before the World Health Organization was even aware of an unusual cluster of pneumonia cases in Wuhan, China?
A new analysis of medical records from UCLA hospitals and clinics suggests the answer might be yes.
Researchers from UCLA and their colleagues at the University of Washington documented an unmistakable uptick in patients seeking treatment for coughs. The increase began the week of Dec. 22, 2019, and persisted through the end of February.
Some of those patients were treated in outpatient centers. Others came to emergency rooms, and some were ultimately admitted to the Ronald Reagan UCLA Medical Center or other hospitals operated by UCLA.
… The researchers didn’t conduct any diagnostic tests, so they can’t say with certainty when doctors first encountered anyone infected with the virus that came to be known as SARS-CoV-2. But if the coronavirus had indeed been spreading under the radar since around Christmas, the pattern of patient visits to UCLA facilities would have looked a lot like what actually happened, they wrote in a study published Thursday in the Journal of Medical Internet Research.
“A significantly higher number of patients with respiratory complaints and diseases starting in late December 2019 and continuing through February 2020 suggests community spread of SARS-CoV-2 prior to established clinical awareness and testing capabilities,” wrote the team led by Dr. Joann Elmore, who is both an internist and professor of health policy and management at UCLA.
Students may earn almost 10% less money over their lives due to Covid-19′s impact on education – CNBC
But it’s not only parents’ income that will suffer due to remote learning. Kids’ potential future income may suffer as well, according to a new study published by the Organisation for Economic Co-operation and Development.
For each full academic year of “corona-induced learning loss,” kids in grades 1-12 could earn see their lifetime earnings drop by just over 9%, according to the OECD study. The loss of one-third of the school year — as kids experienced during school closures from March through May — could lower lifetime earnings by 3%.
That is, “if schools immediately returned to 2019 performance levels,” the report notes. “Disadvantaged students will almost certainly see larger impacts. And, with the forecast of further disruptions in normal school operations, the costs only grow.”
… There are three main theories as to why more education leads to increased income, says Cohodes, who is not involved in the OECD study.
- The human capital theory, which states that what you learn in school is of value in the world. This doesn’t just include subjects you are tested on but also skills you learn from being in class, such as teamwork and problem solving.
- Signaling, which means that if you have a high school diploma or other academic credentials, you are signaling to the job market that you are smart and accomplished.
- Furthering your education expands your social networks, which gives you access to more jobs.
Infectious COVID-19 Can Persist in Gut for Weeks – Medscape
For the first time, researchers detected active and prolonged infection of SARS-CoV-2 virus in the gastrointestinal (GI) tracts of people with confirmed COVID-19. Stool tests were positive among people with no GI symptoms, and in some cases up to 6 days after nasopharyngeal swabs yielded negative results.
The small pilot study suggests a quiescent but active infection in the gut. Stool testing revealed genomic evidence of active infection in seven of the 15 participants tested in one of two hospitals in Hong Kong.
Professors Paul Chan (left), Francis Chan, and Siew Ng of the Centre for Gut Microbiota Research at the Chinese University of Hong Kong.
“We found active and prolonged SARS-CoV-2 infection in the stool of patients with COVID-19, even after recovery, suggesting that coronavirus could remain in the gut of asymptomatic carriers,” senior author Siew C. Ng, MBBS, PhD, told Medscape Medical News.
“Due to the potential threat of fecal-oral transmission, it is important to maintain long-term coronavirus and health surveillance,” said Ng, Associate Director of the Centre for Gut Microbiota Research at the Chinese University of Hong Kong (CUHK).
“Discharged patients and their caretakers should remain vigilant and observe strict personal and toileting hygiene,” she added.
UK’s ‘Moonshot’ mass virus test plan met with skepticism – AP
Health experts on Thursday expressed strong skepticism about the British government’s ambitious plans to carry out millions of coronavirus tests daily in a bid to help people resume normal lives in the absence of a vaccine.
Prime Minister Boris Johnson said Wednesday he wanted to roll out much simpler, faster mass testing “in the near future” to identify people who don’t have the virus so that they can “behave in a more normal way in the knowledge they can’t infect anyone else.” Johnson said people with such negative “passports” could then attend events at places like theaters, and he said he was “hopeful” that the plan will be widespread by springtime.
Johnson made the comments as he announced strict new measures to try to curb a sharp recent rise in COVID-19 cases across Britain. From Monday, social gatherings of more than six people will be banned in England — both indoors and outdoors — and Johnson hinted that such restrictions will potentially remain in place until or through Christmas.
Health professionals were quick to question the mass testing claims, with one expert calling the strategy — known as “Operation Moonshot” — “fundamentally flawed.”
“It is being based on technology that does not, as yet, exist,” said Dr. David Strain, clinical lecturer at the University of Exeter. Johnson’s suggestion of new tests that can give rapid results like a pregnancy test is “unlikely if not impossible” by the spring, he said, and the technology is far from reliable.
“Existing technology has been demonstrated to miss up to one-third of people who have COVID-19 in early disease. After a second test 48 hours later, we still miss over a quarter of people,” he said.
People who reported dining out recently were twice as likely to have COVID-19 as compared with people who had not eaten at a restaurant – CDC
Findings from a case-control investigation of symptomatic outpatients from 11 U.S. health care facilities found that close contact with persons with known COVID-19 or going to locations that offer on-site eating and drinking options were associated with COVID-19 positivity. Adults with positive SARS-CoV-2 test results were approximately twice as likely to have reported dining at a restaurant than were those with negative SARS-CoV-2 test results.
What are the implications for public health practice?
Eating and drinking on-site at locations that offer such options might be important risk factors associated with SARS-CoV-2 infection. Efforts to reduce possible exposures where mask use and social distancing are difficult to maintain, such as when eating and drinking, should be considered to protect customers, employees, and communities.
Which Hospital Workers Face Least COVID Risk? Depends on Whom You Mask – Medpage
Hospital clinicians taking care of the sickest COVID-19 patients were associated with the lowest risk of seropositivity versus those working in other areas of the hospital, and personal protective equipment (PPE) may have played a role, British researchers found.
those in general internal medicine, acute medicine, and housekeeping services had a higher risk of seropositivity, they wrote in Thorax.
They hypothesized varying levels of PPE played a role, as intensive care clinicians and those in designated “high risk areas” of the hospital had access to “enhanced PPE,” including “filtered face piece (class 3)” respirators. FFP3 respirators are said to filter out at least 99% of airborne particles. Surgical masks were recommended for staff in other clinical areas.
“We presumed that intensive care workers were going to have the highest risk,” Richter said in a podcast about the study. “Something like the PPE and the protective equipment the individuals were wearing may well play an important part in this finding.”
But she noted the study was not specifically set up to examine PPE, adding further research is needed to determine if the type of PPE plays a role in infection risk. Some American physicians encouraged N95 masks for all inpatient care during the COVID-19 pandemic, though many organizations say surgical masks are adequate for most healthcare providers.
Whatever Happened To … The Instant Hospitals Built For COVID-19 Patients In Wuhan? – NPR
In February, China pulled off an impressive construction feat that caught the world’s attention: Amid surging cases of COVID-19, China built two hospitals in the pandemic’s epicenter, Wuhan, in under two weeks to isolate and treat COVID-19 patients. Consisting largely of prefabricated rooms and components, the two-story structures were dubbed “instant hospitals.” NPR reported on the facilities just as the first one opened. But now the virus is under control in Wuhan, and life has more or less returned to normal. So, what happened to these “instant hospitals?”
… According to state media, Leishenshan ended up treating a total of 2,011 patients over the two months it was operational. Government officials say there are no plans to demolish the hospitals yet, and they can be “reactivated at any time” if a second wave of infections hits.
“Although the health workers [in these two field hospitals] have returned to their workplaces, the equipment and facilities are still there so that if needed, the workers can be mobilized again and the hospital can be reopened,” says Yanzhong Huang, a senior fellow for global health at the Council on Foreign Relations.
What happens after the pandemic is still unclear, but if the hospitals’ predecessor is any indication, not much.
Persistent Lung Damage Improves Gradually After COVID-19 – Medscape
The vast majority of hospitalized COVID-19 patients show lung damage 6 weeks after discharge, but this proportion drops significantly after 12 weeks, suggesting that the lungs have a self-repair mechanism, researchers report.
“We know from other lung studies that lungs have the potential to recover from inflammation,” said investigator Sabina Sahanic, MD, a clinical PhD student at University Clinic in Innsbruck, Austria. “Specialists knew we’d have to wait some weeks to clarify this and estimate how good the resolution is. And we are very happy to see a good resolution.”
The 86-patient preliminary analysis — believed to be the first prospective study tracking lung and heart outcomes in COVID-19 patients — also showed that shortness of breath is the most common symptom 6 weeks after discharge, affecting 47% of patients, followed by coughing, affecting 15%. At 12 weeks, only 39% of patients were still experiencing shortness of breath, but 15% were still coughing.
“The 12-week timeline is particularly important because in many other lung diseases at this time point, we can estimate resolution or recovery,” Sahanic told Medscape Medical News.
But “we have no definition here of what is long-term,” she said. “We are really early in the pandemic phase, at 3 months, and we do not know how long diseased lungs [from COVID-19] will react to other infections.”
Colleges are now hot spots, as nursing homes and meatpacking plants were earlier in the pandemic. – New York Times
It began as a trickle of coronavirus infections as college students arrived for the fall semester. Soon that trickle became a stream, with campuses reporting dozens, and sometimes hundreds of new cases each day.
Now the stream feels like a flood. In just the past week, a New York Times survey has found, American colleges have recorded more than 36,000 additional infections, bringing the total of 88,000 cases since the pandemic began.
Not all those cases are new, and the increase is partly the result of more schools beginning to report the results of more testing. But The Times survey of 1,600 colleges also shows how widely the contagion has spread, with schools of every type and size, and in every state reporting infections.
Italy is calling back coronavirus survivors in Bergamo. About half say they haven’t fully recovered. – Washington Post
The first wave is over, thousands have been buried, and in a city that was once the world’s coronavirus epicenter, the hospital is calling back the survivors. It is drawing their blood, examining their hearts, scanning their lungs, asking them about their lives.
Twenty people per day, it is measuring what the coronavirus has left in its wake.
“How are you feeling?” a doctor recently asked the next patient to walk in, a 54-year-old who still can’t ascend a flight of steps without losing her breath.
“I feel like I’m 80 years old,” the woman said.
Six months ago, Bergamo was a startling warning sign of the virus’s fury, a city where sirens rang through the night and military trucks lined up outside the public hospital to ferry away the dead. Bergamo has dramatically curtailed the virus’s spread, but it is now offering another kind of warning, this one about the long aftermath, where recoveries are proving incomplete and sometimes excruciating.
… The follow-ups with the once-hospitalized patients are the basis for medical research: Their health records now fill 17 bankers’ boxes, and scientific reports are on the way. Bergamo doctors say the disease clearly has full-body ramifications but leaves wildly differing marks from one patient to the next, and in some cases few marks at all. Among the first 750 patients screened, some 30 percent still have lung scarring and breathing trouble. The virus has left another 30 percent with problems linked to inflammation and clotting, such as heart abnormalities and artery blockages. A few are at risk of organ failure.
Study links coronavirus mortality to air pollution exposure – The Hill
A new study published Friday is the latest linking pollution exposure to a greater risk of dying from the coronavirus.
The study published by IOP found that an increase in the concentration of multiple pollutants from a class known as hazardous air pollutants (HAPs) was associated with a 9 percent increase in COVID-19 mortality.
The study also linked diesel exhaust, soot and smog, as well as substances known as naphthalene and acetaldehyde on their own, to increased coronavirus mortality rates.
Low-income communities and communities of color are more likely to live in areas with greater pollution rates and have also been disproportionately impacted by the pandemic.
The study linked an 0.5 microgram-per-cubic-meter increase in the concentration of diesel exhaust to a 182 percent increase in the mortality rate. It also linked a 0.3-microgram-per-cubic-meter increase of naphthalene to a 791 percent increase in mortality rate.
CDC says Covid-19 death rate is under 1% for everyone but people over 70 – CNN
The US Centers for Disease Control and Prevention said Thursday it had changed the way it was reporting death rates for coronavirus, and will now report the infection fatality ratio by age.
It’s all still based on approximations, and as part of the update the CDC also estimates it’s missing most cases of coronavirus in the US — by a factor of 11.
According to the updated “best estimate” numbers posted on the agency’s website:
- 0.003% of children 18 and younger who are infected with coronavirus die.
- The fatality rate is 0.02% of people aged 20 to 49.
- 0.5% of people aged 50 to 69.
- 5.4% of people 70 and older.
The most dangerous phase of the US Covid-19 crisis may be yet to come – The Guardian
[editor’s note: this is a think piece – not an evidence based post]
April marked the most dramatic and, some would say, dangerous phase of the Covid-19 crisis in the US. Deaths were increasing, bodies were piling up in refrigerated trucks outside hospitals in New York City and ventilators and personal protective equipment were in desperately short supply. The economy was falling off the proverbial cliff, with unemployment soaring to 14.7%.
Since then, supplies of medical and protective equipment have improved. Doctors are figuring out when to put patients on ventilators and when to take them off. We have recognised the importance of protecting vulnerable populations, including the elderly. The infected are now younger on average, further reducing fatalities. With help from the Coronavirus Aid, Relief, and Economic Security (Cares) Act, economic activity has stabilised, albeit at lower levels.
Or so we are being told.
In fact, the more dangerous phase of the crisis in the US may actually be now, not last spring. While death rates among the infected are declining with improved treatment and a more favourable age profile, fatalities are still running at roughly a 1,000 a day. This matches levels at the beginning of April, reflecting the fact that the number of new infections is half again as high.
Mortality, in any case, is only one aspect of the virus’s toll. Many surviving Covid-19 patients continue to suffer chronic cardiovascular problems and impaired mental function. If 40,000 cases a day is the new normal, then the implications for morbidity – and for human health and economic welfare – are truly dire.
As schools reopen, more parents are pulling their children out – CNBC
- As schools reopen for the fall, some families are reconsidering a traditional education.
- One in 10 parents said their child will be home-schooled this year, a number that has doubled since last year.
57 People Face Federal Charges Of Defrauding Coronavirus Relief Program – NPR
The Justice Department’s Criminal Division says it has charged 57 people to date over allegedly defrauding a federal program meant to provide relief to small businesses during the coronavirus pandemic.
The Criminal Division’s acting assistant attorney general, Brian Rabbitt, told reporters that those charged attempted to steal more than $175 million. They actually obtained more than $70 million, he said, and the Justice Department has been to recover or freeze over $30 million.
The Paycheck Protection Program, which was designed to help businesses keep workers on their payroll, was approved by Congress in March as the coronavirus crisis was emerging. Before it closed to new applications last month, according to Rabbitt, it doled out some $525 billion in forgivable loans.
“We allege that many of these defendants took the relief money offered by the PPP and spent it on things having absolutely nothing to do with relief,” Rabbitt said. For example: A Miami man who allegedly obtained almost $4 million in funds and used some of this money to buy a Lamborghini.
Many Employee Concerns Overlooked: Less Than 60% of Organizations Even Surveyed Employees about Readiness to Return to the Workplace – The Conference Board
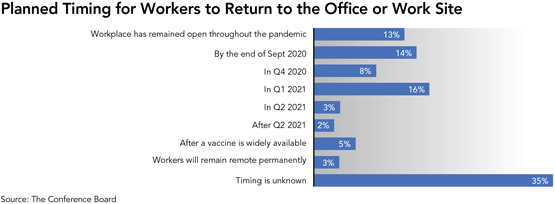
Many businesses hoped to reopen their workplaces after Labor Day, but a new survey of managers and executives suggests a long, uncertain road ahead. 35 percent say the timing of when their companies will reopen the workplace is unknown.
The Conference Board survey also found that only about 60 percent of companies have consulted their workers about their levels of readiness and comfort in returning to the workplace. In addition, despite talk of a looming vaccine and its benefits, just 5 percent say its wide availability would be a significant factor in the timing of a return to the workplace. The findings also reveal that, while most companies have mandated certain protocols for employees arriving at work, only 67 percent are requiring screening, testing, or temperature checks.
The survey polled more than 1,100 businesspersons across 20 US metropolitan statistical areas (MSAs). The respondents – primarily C-suite executives, vice presidents, and senior managers – represent a cross-section of industries. The online survey was fielded from August 19th -26th. Key findings include:
Over a third of companies have not set a date for reopening.
- Over a third of companies surveyed, 35 percent, say their reopening date is still unknown.
- 39 percent of companies plan to reopen by the first quarter of 2021.
- 13 percent of companies have remained open throughout the pandemic.
- The highest levels of uncertainty: Miami (46%), Seattle (43%), San Diego (42%), Washington, DC (41%), and San Francisco (41%).
For reopening, a vaccine is not top of mind.
- Just 5 percent thought the widespread availability of a vaccine would be a significant factor in the timing of a return to the workplace.
- This low ranking likely reflects concern about the viability of a vaccine with a significantly shorter clinical trial time. It also likely reflects concern about the legal implications for any corporate mandate to get the vaccine as a condition for returning.
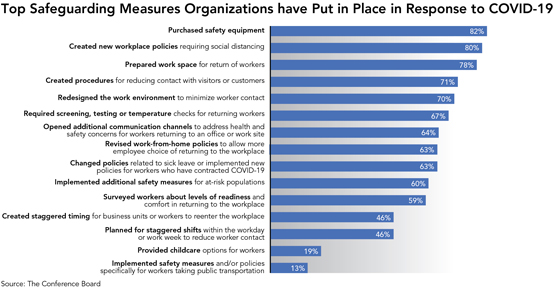
The most and least frequent actions businesses are taking to safeguard their workers:
The most frequent:
- Purchasing safety equipment (e.g., masks, thermometers, contactless entry devices, sanitization devices) (82 percent).
- Creating new workplace policies requiring social distancing (e.g., limiting size of in-person meetings or usage of common areas) (80 percent).
- Preparing workspace for return of workers (e.g., deep cleaning or disinfecting) (78 percent).
The least frequent:
- Providing childcare options for workers (e.g., on-site childcare, flexible scheduling to meet childcare needs) (19 percent).
- Implementing safety measures and/or policies specifically for workers taking public transportation (e.g., requiring more frequent screening or providing extra safety supplies for workers who use public transportation or shared shuttles) (13 percent).
Do employees feel comfortable returning? Only about 60 percent of companies have even checked.
- About 60 percent of businesses chose to survey workers about their levels of readiness and comfort in returning.
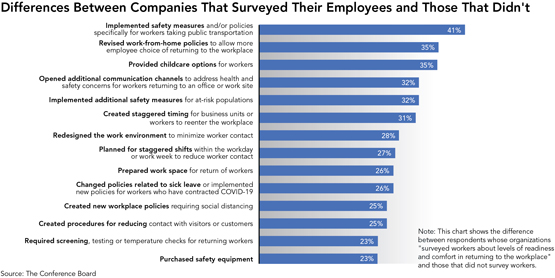
On the upside, those businesses that did survey workers were more likely to put all safeguard measures in place, including top employee concerns.
- “Companies that sought worker sentiment about their comfort levels were more likely to implement safety measures specifically for workers taking public transportation, revise work-from-home policies, and provide childcare options,” said Rebecca Ray, Executive Vice President of Human Capital at The Conference Board. “Notably, these top worker concerns were low on the overall list of safeguards that organizations are implementing, indicating that they are more important to employees than employers may realize. This disconnect reinforces the need for companies to receive buy-in from their most precious resource – their people – especially about matters as consequential as this one.”
Less than half of companies have enacted or plan to enact staggered shifts or staggered timing.
- Despite fairly consistent health organization guidance regarding social distancing, only 46 percent planned for staggered shifts within the workday or work week to reduce worker contact.
- Moreover, only 46 percent plan to create staggered timing for business units or workers to reenter the workplace.
Two-thirds of companies are requiring screening, testing, or temperature checks.
- 67 percent of companies are requiring screening, testing, or temperature checks for returning workers.
- Such actions may not have universal backing due to the fear of litigation – specifically relating to who is asked to come back into the workplace – along with the efficacy of these protocols.
This analysis is a continuation of previous work by The Conference Board. In April 2020, researchers gauged how organizations were reacting to the changing business environment in the context of their workforces.
The following are foreign headlines with hyperlinks to the posts
French new COVID-19 infections at record high, lockdowns feared
Fear and frustration: Europe’s wealthy keep wallets closed
Several European countries have reported increased community transmission of coronavirus infection.
Scientists from Imperial College London said that the prevalence of coronavirus infections doubled every eight days from late August to early September in England, a significant quickening of the spread.
Israel reportedly heads toward nationwide lockdown again
The following are additional national and state headlines with hyperlinks to the posts
Stanford Medical faculty lambaste former colleague and Trump coronavirus advisor Dr. Scott Atlas
Small Study Shows Convalescent Plasma is Safe to Use in Pediatric Patients with COVID-19
Ohio AG Dave Yost thinks Ohio State can sue Big Ten over football cancellation
No Wifi, No AC: Inside the Chaos of 1,400 COVID Cases at The University of South Carolina
U.S. cites Smithfield Foods for failing to protect workers from coronavirus
New York City Public Transit Riders Who Don’t Mask Up Will Face Fines Starting Monday
Fauci: Return to pre-coronavirus normality will be ‘well into 2021’
Couple Together for 50 Years Die From COVID-19 While Holding Hands
At Least 44 9/11 First Responders Believed to Have Died From Coronavirus
College Students Caught Throwing Party, One Says All Attendees Have COVID
Failure to Pass Another Stimulus Bill Could Increase Unemployment: Survey
Getting prisoners in Oregon out of the path of wildfires raises the risk of spreading the virus.
Towns with college students among hottest outbreaks, report says
Fauci says U.S. won’t get back to normal until late 2021
Today’s Posts On Econintersect Showing Impact Of The Pandemic With Hyperlinks
Coronavirus INTERACTIVE Charts
include($_SERVER[‘DOCUMENT_ROOT’].’/pages/coronavirus.htm’); ?>
Analyst Opinion of Coronavirus Data
There are several takeaways that need to be understood when viewing coronavirus statistical data:
- The global counts are suspect for a variety of reasons including political. Even the U.S. count has issues as it is possible that as much as half the population has had coronavirus and was asymptomatic. It would be a far better metric using a random sampling of the population weekly. In short, we do not understand the size of the error in the tracking numbers.
- Just because some of the methodology used in aggregating the data in the U.S. is flawed – as long as the flaw is uniformly applied – you establish a baseline. This is why it is dangerous to compare two countries as they likely use different methodologies to determine who has (and who died) from coronavirus.
- COVID-19 and the flu are different but can have similar symptoms. For sure, COVID-19 so far is much more deadly than the flu. [click here to compare symptoms]
- From an industrial engineering point of view, one can argue that it is best to flatten the curve only to the point that the health care system is barely able to cope. This solution only works if-and-only-if one can catch this coronavirus once and develops immunity. In the case of COVID-19, herd immunity may need to be in the 80% to 85% range. WHO warns that few have developed antibodies to COVID-19. At this point, herd immunity does not look like an option although there is now a discussion of whether T-Cells play a part in immunity [which means one might have immunity without antibodies]
- Older population countries will have a higher death rate.
- There are at least 8 strains of the coronavirus. New York may have a deadlier strain imported from Europe, compared to less deadly viruses elsewhere in the United States.
- Each publication uses different cutoff times for its coronavirus statistics. Our data uses 11:00 am London time. Also, there is an unexplained variation in the total numbers both globally and in the U.S.
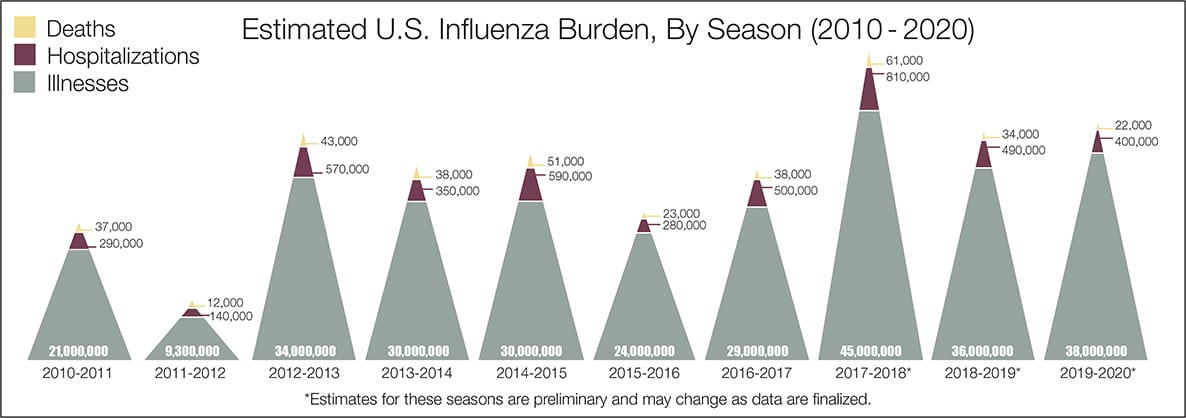
- The real question remains if the U.S. is over-reacting to this virus. The following graphic from the CDC puts the annual flu burden in perspective [click on image to enlarge]. Note that using this data is dangerous as the actual flu cases are estimated and not counted – nobody knows how accurate these guesses are.
What we do not know about the coronavirus [actually there is little scientifically proven information]. Most of our knowledge is anecdotal, from studies with limited subjects, or from studies without peer review.
- How many people have been infected as many do not show symptoms?
- Masks do work.
- Do we develop lasting immunity to the coronavirus? Another coronavirus – the simple cold – does not develop long term immunity.
- To what degree do people who never develop symptoms contribute to transmission?
- The US has scaled up coronavirus testing – and the accuracy of the tests has been improving. However, if one loses immunity – the coronavirus testing value is reduced.
- Can children widely spread coronavirus? [current thinking is that they are becoming a major source of the pandemic spread]
- Why have some places avoided big coronavirus outbreaks – and others hit hard?
- What effect will the weather have? At this point, it does not seem hot weather slows this coronavirus down – and it seems air conditioning contributes to its spread.
- Outdoor activities seem to be a lower risk than indoor activities.
- Can the world really push out an effective vaccine in 12 to 18 months?
- Will other medical treatments for Covid-19 ease symptoms and reduce deaths? So far only one drug (remdesivir) is approved for treatment.
- A current scientific understanding of the way the coronavirus works can be found [here].
Heavy breakouts of coronavirus have hit farm workers. Farmworkers are essential to the food supply. They cannot shelter at home. Consider:
- they have high rates of the respiratory disease [occupational hazard]
- they travel on crowded buses chartered by their employers
- few have health insurance
- they cannot social distance and live two to four to a room – and they eat together
- some reports say half are undocumented
- they are low paid and cannot afford not to work – so they will go to work sick
- they do not have access to sanitation when working
- a coronavirus outbreak among farmworkers can potentially shutter entire farm
The bottom line is that COVID-19 so far has been shown to be much more deadly than the data on the flu. Using CDC data, the flu has a mortality rate between 0.06 % and 0.11 % Vs. the coronavirus which to date has a mortality rate of 4 % [the 4% is the average of overall statistics – however in the last few months it has been hovering around 1.0%] – which makes it between 10 and 80 times more deadly. The reason for ranges:
Because influenza surveillance does not capture all cases of flu that occur in the U.S., CDC provides these estimated ranges to better reflect the larger burden of influenza.
There will be a commission set up after this pandemic ends to find fault [it is easy to find fault when a once-in-a-lifetime event occurs] and to produce recommendations for the next time a pandemic happens. Those that hate President Trump will conclude the virus is his fault.
Resources:
- Get the latest public health information from CDC: https://www.coronavirus.gov .
- Get the latest research from NIH: https://www.nih.gov/coronavirus.
- Find NCBI SARS-CoV-2 literature, sequence, and clinical content: https://www.ncbi.nlm.nih.gov/sars-cov-2/.
- List of studies: https://icite.od.nih.gov/covid19/search/#search:searchId=5ee124ed70bb967c49672dad
include(“/home/aleta/public_html/files/ad_openx.htm”); ?>