from the Congressional Budget Office
The CBO released The 2013 Long-Term Budget Outlook. In that report, CBO projects that budget deficits, although projected to decline over the next few years, would gradually rise again under current law, mainly because of increasing interest costs and growing spending for Social Security and the government’s major health care programs—Medicare, Medicaid, the Children’s Health Insurance Program (CHIP), and the subsidies that will be provided starting in 2014 through the newly established health insurance exchanges (see the figure below). This post will provide more detail about the outlook for health care spending.

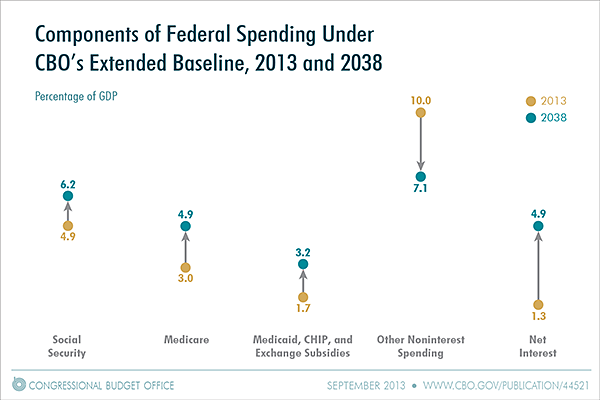
How Has Spending For The Major Health Care Programs Changed Over Time And What Are CBO’s Long-Term Projections Of Spending For Those Programs?
Although spending for health care in the United States has grown more slowly in recent years than it had previously, high and rising levels of such spending continue to pose a challenge not only for the federal government’s two major health insurance programs, Medicare and Medicaid, but also for state and local governments, businesses, and households. Measured as a share of economic output, federal spending for Medicare (net of what are termed offsetting receipts, which mostly consist of premiums paid by beneficiaries) and Medicaid rose from 1.8 percent of gross domestic product (GDP) in fiscal year 1985 to 4.6 percent in 2012. Total national spending on health care services and supplies increased from 4.6 percent of GDP in calendar year 1960 to 9.5 percent in 1985 and to 16.4 percent in 2011, the most recent year for which such data are available.
Under CBO’s extended baseline, which generally relies on an assumption that current law remains in place, federal spending on the government’s major health care programs is expected to rise substantially relative to GDP (see the figure below). Specifically, net federal spending for those programs (that is, spending net of offsetting receipts for Medicare) would grow from an estimated 4.6 percent of GDP in fiscal year 2013 to 8.0 percent in 2038; in that year, 4.9 percent of GDP would be devoted to net spending on Medicare and 3.2 percent would be spent on Medicaid, CHIP, and the exchange subsidies. Beyond 2038, CBO projects, federal health care spending would continue to climb relative to GDP but at a slower rate than has been sustained historically.
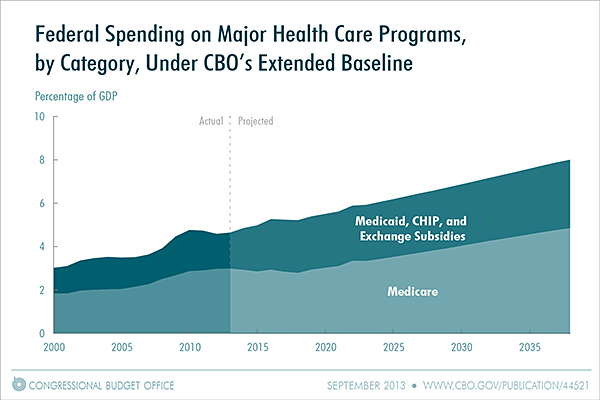
What Factors Are Affecting Growth In Health Care Spending?
Health care spending per person has grown faster, on average, than the nation’s economic output per person since calendar year 1985, even after the recent slowdown is factored in. On the basis of a calculation that gives greater weight to more recent years, CBO estimates that growth in health care spending per person (after adjusting for demographic changes) has outpaced growth in GDP per capita by an average of 1.5 percent per year since 1985. Key factors contributing to that faster growth have been the emergence and increasing use of new medical technologies, rising personal income, and the expanding scope of health insurance coverage. Factors that have restrained growth during that period, at least temporarily, include the spread of managed care plans in the 1990s and the recent economic recession, as well as legislated changes in Medicare’s payment policies such as those introduced in the Balanced Budget Act of 1997.
The growth of health care spending cannot exceed economic growth indefinitely, because if it did, total spending on health care would eventually account for all of the country’s economic output—an impossible outcome. Instead, over time, people will try to limit their spending for health care in order to maintain their consumption of other goods and services. Private insurers and employers will adjust the insurance coverage they offer, the benefits they provide, and the amounts and nature of their payments to health care providers. In addition, state governments—which pay a large share of Medicaid’s costs and have considerable influence on those costs—will limit the growth of spending for health care in order to manage their budgets. Those reactions to cost pressures will increase the incentives for health care providers to invest in cost-reducing technologies and to increase efficiency. Thus, even in the absence of changes in federal law, growth in per capita spending on Medicaid and on health care financed through the private sector will gradually slow. The rate of growth of Medicare spending per beneficiary is also likely to slow, though to a lesser extent, even without changes in federal law—reflecting changes in medical practices common to all patients, payment rate changes allowed or required under current law, and the increasing pressure of premiums and cost-sharing amounts, such as copayments and deductibles, on enrollees’ finances.
However, quantifying the extent to which the rate of growth of health care spending will decline under current law is difficult. The growth of such spending relative to the growth of the economy has varied greatly from year to year during the past several decades, so projections of the difference in growth rates in the future are very uncertain. As the projection period lengthens, the uncertainties mount because the likelihood of significant changes in medical practices and technology increases.
A particular challenge currently is estimating the extent to which the recent slowdown in growth can be attributed to temporary factors like the recession or instead reflects more enduring developments. Studies have generally concluded that a portion of the observed reduction in growth cannot be linked directly to the weak economy, and CBO’s own analysis has found no link between the recession and slower growth in spending for Medicare. Accordingly, over the past few years, CBO has substantially reduced its projections of spending on Medicare and
Medicaid during the coming decade and slightly lowered its estimate of the underlying rate of growth for health care spending per person for the country as a whole. CBO’s estimate of that underlying rate takes into account spending trends since 1985 but gives greater weight to the recent experience; because of the pressures to constrain spending growth, the underlying rate is projected to decline gradually in the long run.
In contrast, federal spending for health care will be pushed up in the future by a sharp increase in the number of people receiving benefits from government programs. That increase can be attributed to two main factors. The first is the aging of the population—in particular, the aging of the baby-boom generation (people born between 1946 and 1964)—which will increase the number of people receiving benefits from Medicare by more than one-third over the next decade. The second is the expansion of federal support for health insurance under the Affordable Care Act, which will significantly increase the number of people receiving benefits from Medicaid and make other people eligible for subsidies for health insurance purchased through exchanges.
Author: Julie Topoleski is an analyst in CBO’s Health, Retirement, and Long-Term Analysis Division.
An Overview Of The Medicare Program
In fiscal year 2013, Medicare will provide federal health insurance to 52 million people who are elderly or disabled or have end-stage renal disease. (The elderly make up about 85 percent of enrollees.) People become eligible for Medicare on the basis of age when they reach 65; disabled individuals generally become eligible for the program 24 months after they qualify for benefits under Social Security’s Disability Insurance program. In general, a beneficiary or the beneficiary’s spouse must have worked and paid sufficient Medicare payroll taxes for a specified number of years—10 years for most elderly beneficiaries.
The Medicare program provides a specified set of benefits. Hospital Insurance (HI), or Medicare Part A, primarily covers inpatient services provided by hospitals as well as care in skilled nursing facilities, home health care, and hospice care. Part B mainly covers services provided by physicians and other practitioners and by hospitals’ outpatient departments, and Part D provides a prescription drug benefit. Most enrollees in Medicare are in the traditional fee-for-service program, in which the federal government pays for covered services directly, but enrollees can instead obtain coverage for Medicare benefits through a private health insurance plan under Part C of the program, known as Medicare Advantage. In 2012, net spending for Medicare (that is, with the offsetting receipts that mostly consist of beneficiaries’ payments of premiums taken into account) was $466 billion. Gross spending for Medicare was $551 billion in that year. (Those amounts do not include several billion dollars of administrative costs subject to appropriation.)
The various parts of the program are financed in different ways. Part A benefits are financed primarily by a payroll tax (2.9 percent of all taxable earnings), the revenues from which are credited to the HI trust fund. Beginning in 2013, an additional 0.9 percent tax on earnings over $200,000 ($250,000 for married couples) is also being credited to the trust fund. For Part B, premiums paid by beneficiaries cover just over one-quarter of outlays, and the government’s general funds cover the rest. Federal payments to private insurance plans under Part C are financed by a blend of funds from Parts A and B. Enrollees’ premiums under Part D are set to cover about one-quarter of the cost of the basic prescription drug benefit, although many low-income enrollees pay no premiums; general funds from the Treasury cover most of the remaining cost. Altogether, in calendar year 2012, receipts from the payroll tax were equal to about 36 percent of gross federal spending on Medicare, beneficiaries’ premiums were equal to about 12 percent, and general funds allocated to the program’s trust funds amounted to about 37 percent; the trust funds are also credited with money from other sources.
Cost-sharing requirements in Medicare vary widely, and the program does not set an annual cap on the amount of health care costs for which beneficiaries are responsible. However, the vast majority of beneficiaries who receive care in the fee-for-service portion of Medicare have supplemental insurance that covers many or all of the program’s cost-sharing requirements. According to one recent study, the most common sources of supplemental coverage in 2009 were plans for retirees offered by former employers (held by 43 percent of beneficiaries in the fee-for-service part of Medicare), individually purchased medigap policies (29 percent of beneficiaries), and Medicaid (17 percent of beneficiaries). Many people covered through Medicare Advantage receive additional benefits or purchase additional coverage that provides some supplemental benefits.
A number of provisions of law will constrain the rates that Medicare pays to providers of health care in the future:
- Payments for physicians’ services in Medicare are governed by the sustainable growth rate mechanism. Under current law, those payment rates will be reduced by about 25 percent in January 2014 and by small amounts in subsequent years, CBO projects. In recent years, legislation has been enacted to block similar reductions that were scheduled to occur.
- The Affordable Care Act (ACA) contains numerous provisions that, on balance, will reduce federal spending on Medicare. The provisions with the greatest effect on the projected growth of Medicare spending impose permanent reductions in the annual updates to Medicare’s payment rates for many types of health care providers (other than physicians) in the fee-for-service portion of the program.
- The ACA also established an Independent Payment Advisory Board (IPAB), which will be required to submit a proposal to reduce Medicare spending in certain years if the rate of growth in spending per enrollee is projected to exceed specified targets. The proposal—or an alternative proposal submitted by the Secretary of Health and Human Services if the board does not submit a qualifying proposal—must achieve a specified amount of savings in the year it is implemented while not increasing spending in the succeeding nine years by more than the amount of those first-year savings. The ACA places a number of limitations on the actions available to the IPAB, including a prohibition against modifying Medicare’s eligibility rules or reducing benefits.
- The Budget Control Act of 2011, as subsequently amended, specifies automatic procedures—sequestration, or the cancellation of funding—that will reduce most Medicare payments to providers for services furnished from April 2013 to March 2022. Under that act, most of Medicare’s spending will be subject to a 2 percent reduction.
To learn more, see The 2013 Long-Term Budget Outlook; you can also visit Medicare page for a complete set of CBO’s work on this topic.
Authors: Tom Bradley is Chief of the Health Systems and Medicare Cost Estimates Unit in CBO’s Budget Analysis Division. Julie Topoleski is an analyst in CBO’s Health, Retirement, and Long-Term Analysis Division.
Source: An Overview Of The Medicare Program
An Overview Of The Medicaid Program
Medicaid is a joint federal-state program that pays for health care services for low-income individuals, including pregnant women, children, and parents and other caretaker relatives, as well as elderly and disabled individuals. As a result of the Affordable Care Act (ACA) and a subsequent Supreme Court ruling, each state has the option to expand eligibility for Medicaid beginning in calendar year 2014 to all nonelderly adults with income below 138 percent of the federal poverty guidelines (commonly referred to as the federal poverty level, or FPL). The people who will be newly eligible for Medicaid consist primarily of nonelderly adults with low income. Most children and pregnant women in low-income families qualify for Medicaid and the Children’s Health Insurance Program under prior law. Some parents of those children also qualify for Medicaid, although the income thresholds vary by state.
The federal government’s share of Medicaid’s spending for benefits varies among the states. That share historically has averaged about 57 percent. Beginning in calendar year 2014, the federal government will pay all of the costs of covering enrollees newly eligible under the ACA’s coverage expansion. From 2017 to 2020, the federal share of that spending will decline gradually to 90 percent, where it will remain thereafter. According to CBO’s estimates, those changes will result in a federal share of Medicaid’s spending that averages 60 percent by 2020.
In fiscal year 2012, federal spending for Medicaid was $251 billion, of which $223 billion covered benefits for enrollees. (In addition to benefits, Medicaid’s spending included payments to hospitals that treat a “disproportionate share” of low-income patients, costs for the Vaccines for Children program, and administrative expenses.) According to the Centers for Medicare & Medicaid Services, states spent $160 billion on Medicaid in calendar year 2011, the most recent year for which data are available.
States administer their Medicaid programs under federal guidelines that specify a minimum set of services that must be provided to certain categories of low-income individuals. Required services include inpatient and outpatient hospital services, services provided by physicians and laboratories, and nursing home and home health care. To be eligible for Medicaid, a person must have a low income and generally only a few assets—although the financial limits vary depending on the basis for an enrollee’s eligibility. Groups that must be eligible include children in low-income families and families who would have qualified for the former Aid to Families with Dependent Children program, certain other children in low-income families and pregnant women, and most elderly and disabled individuals who qualify for the Supplemental Security Income program.
Subject to those requirements and other statutory limits, states have flexibility in administering the Medicaid program and determining its scope. States may choose to make additional groups of people eligible (such as individuals with income above the standard eligibility limits and those who have high medical expenses relative to their income) or to provide additional benefits (such as coverage for prescription drugs and dental services), and they have exercised those options to varying degrees. Moreover, many states seek and receive federal waivers that allow them to provide benefits and cover groups that would otherwise be excluded. As a result, the program’s rules are complex, and it is difficult to generalize about the types of enrollees covered, the benefits offered, and the cost sharing required. By one estimate, federal and state expenditures on optional populations and benefits accounted for about 60 percent of the Medicaid program’s total spending in 2007.
About 72 million people will be enrolled in Medicaid at some point during 2013, CBO estimates; the average enrollment over the course of the year will be about 57 million. Those two ways of measuring enrollment yield divergent estimates because many people are enrolled in Medicaid for only part of the year.
Currently, almost half of Medicaid’s enrollees are children in low-income families, and just under one-third are either the parents of those children or low-income pregnant women. The elderly and disabled constitute the remaining almost one-quarter of enrollees. Expenses tend to be higher for beneficiaries who are elderly and disabled, many of whom require long-term care, than for other beneficiaries. In 2012, about 32 percent of federal Medicaid spending for benefits was for long-term services and supports, which include institutional care provided in nursing homes and certain other facilities as well as care provided in a person’s home or in the community. Overall, the elderly and disabled account for almost two-thirds of Medicaid’s payments for benefits.
To learn more, see The 2013 Long-Term Budget Outlook; you can also visit our Medicaid page for a complete set of CBO’s work on this topic.
Authors: Jean Hearne is Chief of the Low-Income Health Programs and Prescription Drugs Cost Estimates Unit in CBO’s Budget Analysis Division. Julie Topoleski is an analyst in CBO’s Health, Retirement, and Long-Term Analysis Division.
Source: An Overview Of The Medicaid Program
A Premium Support System For Medicare: Analysis Of Illustrative Options
Over the past two decades, numerous proposals have been advanced for the establishment of a premium support system for Medicare. Under such a program, beneficiaries would purchase health insurance from one of a number of competing plans, and the federal government would pay part of the cost of the coverage. The various proposals have differed in many respects, including the way in which the federal contribution would be set and how that contribution might change over time.
This CBO report presents a preliminary analysis of the ways two illustrative options for a premium support system would affect federal spending and beneficiaries’ choices and payments. The agency has developed significant new tools to analyze such a system in greater depth than in the past; the specifications of the options examined here also differ from those CBO analyzed previously. As the agency refines its modeling approach and considers alternative options for a premium support system, its findings could change. CBO’s analysis to date, as summarized in the figure below, indicates the following:
- Both options for premium support considered here would reduce federal spending for Medicare net of beneficiaries’ premiums and other offsetting receipts.
- Under the second-lowest-bid option, the option with the greater reduction in net federal spending, beneficiaries’ premiums and total payments for Medicare’s Part A and Part B benefits would each be higher on average than they would be under current law. (Total payments consist of premiums and out-of-pocket costs for deductibles, copayments, and coinsurance.) Under the average-bid option, the option with the smaller reduction in net federal spending, those amounts would each be lower on average than they would be under current law.
- Under both options, combined spending by the federal government and by beneficiaries (that is, premiums and out-of-pocket costs) would be less than that if current law remained in place.
- Under both options, effects on premiums and total payments for some beneficiaries would differ greatly from the national averages. In particular, in most regions, the premiums and total payments of beneficiaries enrolled in the fee-for-service program would be higher than they would be under current law.
- Alternative specifications for key features of a premium support system would yield different results.
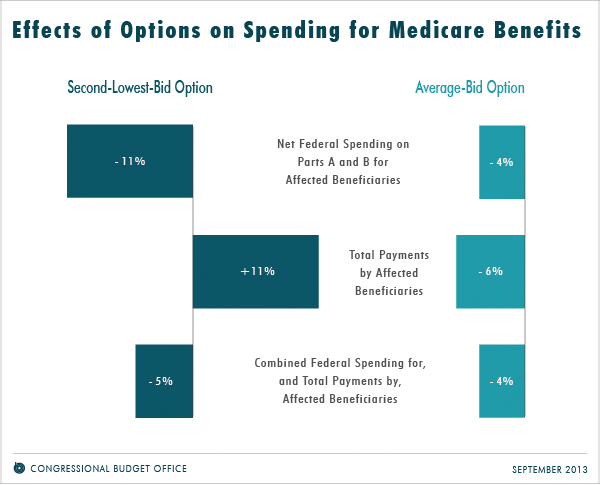
Source: A Premium Support System For Medicare: Analysis Of Illustrative Options
************************






