by Timothy Taylor, Conversable Economist
We know several facts about US life expectancy with a high degree of confidence. Overall, life expectancy is rising: indeed, it is rising for every age group. However, there have long been gaps in life expectancy between various groups, like those with higher and lower income levels.

What we don’t know about life expectancy with a high degree of confidence, and are still sorting out, is how the changes in life expectancy across groups are evolving. Janet Currie and Hannes Schwandt tackle this question in “Mortality Inequality: The Good News from a County-Level Approach,” published in the Spring 2016 issue of the Journal of Economic Perspectives.
Currie and Schwandt provide this quick overview of recent studies:
However, this overall decline in mortality rates has been accompanied by prominent recent studies highlighting that the gains have not been distributed equally (for example, Cutler, Lange, Meara, Richards-Shubik, and Ruhm 2011; Chetty et al. 2015; National Academies of Science, Engineering, and Medicine (NAS) 2015; Case and Deaton 2015). Indeed, several studies argue that when measured across educational groups and/or geographic areas, mortality gaps are not only widening, but that for some US groups, overall life expectancy is even falling (Olshansky et al. 2012; Wang, Schumacher, Levitz, Mokdad, and Murray 2013; Murray et al. 2006). It seems to have become widely accepted that inequality in life expectancy is increasing.
But Currie and Schwandt marshall evidence that is arguably more representative than what has been used in the previous studies to argue that in many dimensions, the inequality of life expectancy across various groups is either declining or not changing by much.
One of the issues here is that many sources of data on mortality rates don’t include measures of income. As an example of the issues here, I discussed the NAS study about growing inequality of life expectancy by income on this blog last September. However, that study (and several others) are based on the Health and Retirement Survey, which looks only at people over age 50. Indeed, every six years it chooses a sample of 50 year-olds and then tracks that sample every two years. It’s wonderful data for studying certain choices of this population, and it does include mortality rates and past income. But the entire sample is 20,000 people over the age of 50, so it’s tricky to project back to life expectancies at earlier ages and to do detailed comparisons across groups. The authors write:
“For example, Chetty et al. (2015) use mortality at age 40 to 63 to estimate income-specific trends in life expectancy, while NAS (2015) uses mortality at age 50 to 78, an approach that by construction does not consider developments at younger ages.”
Those who want more detail on difficulties comparing mortality rates by group can go through the Currie and Schwandt article. Here, I want to focus on the county-level approach that they take. Detailed data on mortality rates by age, gender, race is available at the county level. We also have census data on poverty rates by county, median income by county, and other variables. The authors take three years: 1990, 2000, and 2010. They rank the counties in that year according to a certain factor–like poverty rates–and then look at how life expectancies varied across countries. By doing this exercise in 1990, 2000, and 2010, they can look at how inequality of life expectancy is varying over time.
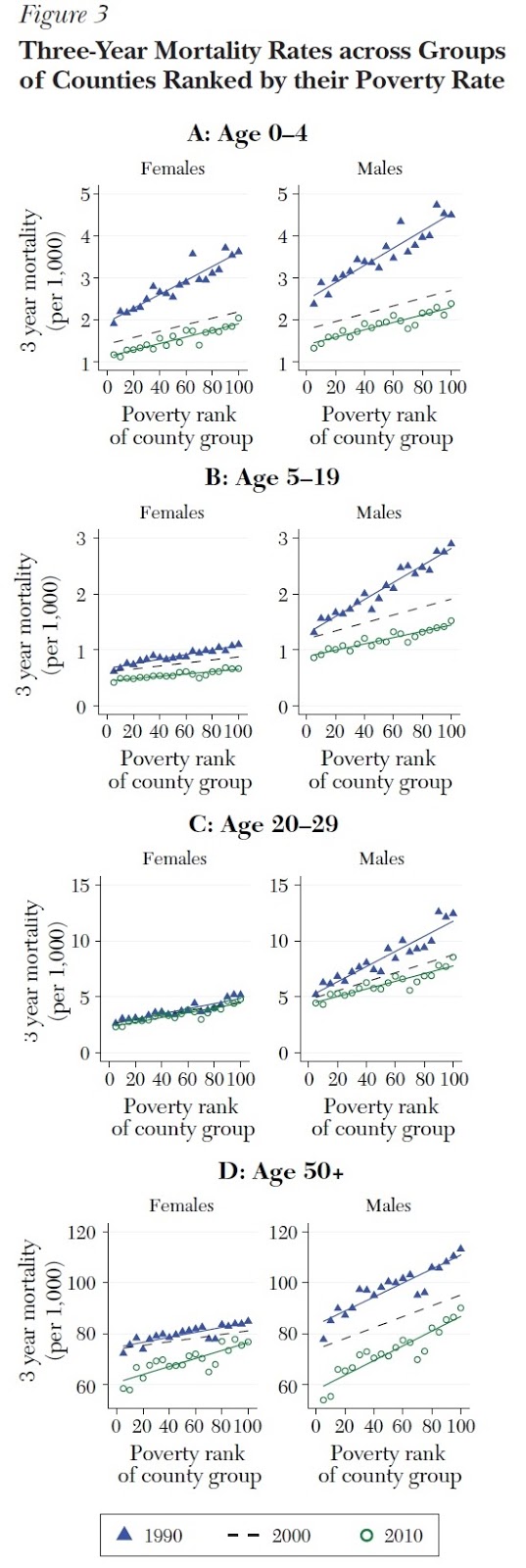
Here’s a sample of the results. Each pair of figures is divide up by age group and by gender. Focus on the upper-left figure for a moment. The blue triangles show the county-level mortality rate for females age 0-4 in counties ranging from the lowest poverty rates up to the highest percentile of poverty rates. To be specific there are 20 blue triangles, one for each five percentiles of the poverty distribution (that is, percentiles 1-5, 6-10, and so on up to 96-100). The blue line is a best-fit line for the blue triangles, and the upward slope shows that counties with higher poverty also have higher mortality rates. The green circles show estimates across counties for the year 2010, and the green line is a best-fit line for 2010. The dashed line is a best-fit line for 2000, but to keep the figures from getting to messy, the separate points aren’t shown for 2000. Overall mortality rates fell from 1990 to 2010. Also, the slope of the green line is flatter than the slope of the blue line, which means that females in the 0-4 age group in high-poverty countries had closed the mortality gap to some extent with those in low-poverty countries.
When you look across these kinds of figures, you see variation across age groups in the size of the mortality decline: that is, the gap between the green and blue lines. You also see differences in how the slope of the mortality lines has changed: for the youngest age groups (which remember were not well-represented in the data from earlier studies), inequality of mortality has decreased, but for women in the 50+ age group, the level of mortality has dropped (green line lower than blue line) but the inequality of mortality is greater (green line steeper than blue line).
If you know anything about academic researchers, you can imagine how Currie and Schwandt work through this kind of data with care and attention. For example, you can rank counties in other ways, like median income or high school dropouts or even the starting level of life expectancy. You can break down the mortality rates by race/ethnicity as well as by age and gender. Here are a few of the conclusions that emerge.
- “We find that inequality in mortality has fallen greatly among children. It is worth emphasizing that the reductions in mortality among African Americans, especially African-American males of all ages, are stunning and that is a major driver of the overall positive picture. This positive finding has been largely neglected in much of the discussion of overall mortality trends.” The authors point out that good health earlier in life is somewhat predictive of good health later in life, so improved mortality among children is good news in both the short run and the long run.
- The changes in inequality of mortality aren’t being primarily driven by the rise of income inequality. There are lots of population segments where income inequality is up an mortality inequality is down. Moreover, as the authors point out, even the direction of causality from income inequality to health problems is questionable; instead, the direction of causality is often that poor health status leads to lower income levels. The drivers of mortality changes across groups probably have more to do with the rate of change in habits (smoking, obesity, perhaps opioids), as well as public policy changes over the last two decades affecting nutrition and access to health care.
- “Although our overall message is more positive than some earlier studies, we do find an alarming stagnation in mortality among white women aged 20 to 49.”
- Changes in smoking rates are probably part of the story here. Men had higher smoking rates than women, but then decreased those smoking rates more dramatically. This pattern probably explains why mortality gains among older women look relatively small (and even negative for some specific groups), and may also explain the greater inequality of mortality rates across counties by poverty level.
Here’s how Currie and Schwandt conclude:
“It sometimes seems as if the research literature on mortality is compelled in some way to emphasize a negative message, either about a group that is doing less well or about some aspect of inequality that is rising. … We believe that a balanced approach to the mortality evidence, which recognizes real progress as well as areas in need of improvement, is more likely to result in sensible policymaking. After all, emphasizing the negative could send the message that “nothing works,” especially in the face of seemingly relentless increases in income inequality. We have emphasized considerable heterogeneity in the evolution of mortality inequality by age, gender, and race. Going forward, identifying social policies that have helped the poor and reduced mortality inequality is an important direction for future research. Similarly, understanding the reasons that some groups and age ranges have seen stagnant mortality rates will be important for mobilizing efforts to reduce inequality in mortality and improve the health of the poor.”
(Full disclosure: I’ve labored in the fields as the Managing Editor of the JEP for 30 years. All articles in JEP, both current and back to the first issue, are freely available online compliments of the American Economic Association.)