Written by Steven Hansen
The U.S. new cases 7-day rolling average is 8.6 % lower than the 7-day rolling average one week ago. U.S. deaths due to coronavirus are now 7.3 % lower than the rolling average one week ago. At the end of this post is a set of interactive graphs and tables for the world and individual States – as well as today’s headlines which include;
- Total U.S. cases of coronavirus now exceed 6 million
- High percentage of frontline healthcare workers who have Covid-19 may not know they have it
- Young workers at risk of financial exhaustion due to coronavirus pandemic
- Cheap, at-home coronavirus tests exist — why aren’t we using them?
- U.S. Will Revive Global Virus-Hunting Effort Ended Last Year
- Remdesivir Receives U.S. Food and Drug Administration Emergency Use Authorization for the Treatment of Patients With Moderate COVID-19
- A Nevada man became the first person in U.S. to catch coronavirus twice, and notably, the second time was worse
- Cloth masks do protect the wearer – breathing in less coronavirus means you get less sick
- Teen and children hospitalizations, deaths from coronavirus increasing: report
- 193 passengers and crew ordered to self isolate after seven people on holiday flight contract coronavirus

My continuing advice is to continue to wash your hands, wear masks, and maintain social distancing. No handwashing, mask, or social distancing will guarantee you do not get infected – but it sure as hell lowers the risk in all situations. In addition, certain activities are believed to carry higher risk – like being inside in air conditioning and removing your mask (such as restaurants, around your children/grandchildren, bars, and gyms). It is all about viral load – and outdoor activities are generally very safe.
The daily number of new cases in the U.S. is remaining stubbornly and embarrassedly high.
The following graphs show the 7-day rolling average for new coronavirus cases and deaths have been updated through 31 August 2020:


z coronavirus.png
Coronavirus Statistics For 31 August 2020 |
| U.S. Only | Global | U.S Percentage of Total | ||||
| Today*** | Cumulative | Today*** | Cumulative | Today | Cumulative | |
| New Confirmed Cases | 42,078 | 6,000,000 | 256,115 | 25,250,000 | 16.4% | 23.8% |
| Deaths** | 290 | 183,069 | 3,687 | 846,841 | 7.9% | 21.6% |
| Mortality Rate | 0.7% | 3.1% | 1.4% | 3.4% | ||
total COVID-19 Tests per 1,000 people | 1.58* | 253.47* | ||||
* as of 28 Aug 2020
** evidently several States included “probable” deaths today in the number
*** red color indicates record number
Coronavirus News You May Have Missed
High percentage of frontline healthcare workers who have Covid-19 may not know they have it – CNN
Many frontline health care workers who care for Covid-19 patients may be infected and not even know it, researchers led by the Centers for Disease Control and Prevention reported Monday. And because the infections are undetected, they can potentially be spread to patients, coworkers, and others in the community.
Their survey of more than 3,200 health workers found 6% had antibodies to coronavirus, indicating they had been infected with the virus. But 69% of them had never been diagnosed with such an infection, 44% did not believe they had ever been infected and 29% said they never had any symptoms.
“A high proportion of SARS-CoV-2 infections among healthcare personnel appear to go undetected,” the team at academic medical centers across the country, including the CDC Covid-19 Response Team, wrote in the CDC’s weekly report.
Young workers at risk of financial exhaustion due to coronavirus pandemic – CNBC
- The coronavirus pandemic has added new financial stress to young workers, 85% of whom said they feel pushed to the limit with regard to juggling work and other responsibilities.
- Many said they are “living like they are broke” rather than above their means.
- Though they may be tempted to let budgeting and financial planning take a back seat, it could be a good time to seek professional help.
Cheap, at-home coronavirus tests exist — why aren’t we using them? – The Hill
Paper antigen strips should be the preferred method of COVID-19 testing. They’re cheap, accessible and, most importantly, fast. The technology works by testing for fragments of viral proteins in an individual’s nasal cavity or saliva, but can be administered in a non-laboratory setting (think a home, school, workplace) and display a positive or negative result within 10 to 15 minutes, much like a pregnancy test. This would enable us to identify who is infectious, as the antigen test is accurate when the viral load is high enough for a person to be contagious. The possibility of widespread rapid testing can bring our schools, workplaces and nation back up to speed without endangering millions of high-risk individuals.
This is not some pie-in-the-sky idea; these are real solutions that exist right now and should be a central part of our ongoing COVID-19 response. I sent a letter to FDA Commissioner Dr. Stephen Hahn urging him to revise guidance for non-laboratory rapid antigen tests, which would allow more paper antigen tests to receive EUAs. In the interest of public health, time is of the essence and revised guidance would jumpstart production and enable Congress to take funding action to get these tests into people’s homes for daily use.
America has shown incredible resilience in the face of COVID-19. Many of you have stayed home to care for children and limit contact with friends and many of you have continued going to work to care for the sick and keep our food supply chain up and running. In just a few months, we went from knowing next to nothing about the virus to performing more than 70 million tests in the U.S. Yet we are far from finished, and if we want to move the country into the next phase of recovery, we require creative solutions. The evidence is clear: antigen testing works, and therefore must be part of this solution.
U.S. Will Revive Global Virus-Hunting Effort Ended Last Year – New York Times
A federal agency is resurrecting a version of Predict, a scientific network that for a decade watched for new pathogens dangerous to humans. Joe Biden has also vowed to fund the effort.
A worldwide virus-hunting program allowed to expire last year by the Trump administration, just before the coronavirus pandemic broke out, will have a second life — whatever the outcome of the presidential election.
Joseph R. Biden Jr. has promised that, if elected, he will restore the program, called Predict, which searched for dangerous new animal viruses in bat caves, camel pens, wet markets and wildlife-smuggling routes around the globe.
The expiration of Predict just weeks before the advent of the pandemic prompted wide criticism among scientists, who noted that the coronavirus is exactly the sort of catastrophic animal virus the program was designed to head off.
Expands Previous Authorization of Veklury to Treat Hospitalized Patients with COVID-19 Regardless of Oxygen Status
The U.S. Food and Drug Administration (FDA) expanded the Emergency Use Authorization (EUA) enabling use of the investigational antiviral Veklury® (remdesivir) to treat all hospitalized patients with COVID-19, in addition to the previous authorization for patients hospitalized with severe COVID-19. The expanded EUA is based on results from the Phase 3 SIMPLE trial evaluating Veklury in hospitalized patients with moderate COVID-19 pneumonia, as well as results from the National Institute of Allergy and Infectious Diseases (NIAID) ACTT-1 trial in hospitalized patients with a range of disease severity.
“With the growing understanding of the utility of Veklury to help improve outcomes for a range of patients with COVID-19, we welcome the FDA’s decision to expand emergency use authorization,” said Merdad Parsey, MD, PhD, Chief Medical Officer, Gilead Sciences. “As we learn more about COVID-19 and we further establish the efficacy and safety profile of Veklury, we see benefit to making the drug available to patients at earlier stages of the disease. Today’s action by the FDA enables physicians to consider a broader range of eligible patients to potentially receive Veklury.”
A Nevada man became the first person in U.S. to catch coronavirus twice, and notably, the second time was worse. – Stat
Immunologists had expected that if the immune response generated after an initial infection could not prevent a second case, then it should at least stave off more severe illness. That’s what occurred with the first known reinfection case, in a 33-year-old Hong Kong man.
… Still, despite what happened to the man in Nevada, researchers are stressing this is not a sky-is-falling situation or one that should result in firm conclusions. They always presumed people would become vulnerable to Covid-19 again some time after recovering from an initial case, based on how our immune systems respond to other respiratory viruses, including other coronaviruses. It’s possible that these early cases of reinfection are outliers and have features that won’t apply to the tens of millions of other people who have already shaken off Covid-19.
… some 48 days later, the man started experiencing headaches, cough, and other symptoms again. Eventually, he became so sick that he had to be hospitalized and was found to have pneumonia.
Researchers sequenced virus samples from both of his infections and found they were different, providing evidence that this was a new infection distinct from the first.
Cloth masks do protect the wearer – breathing in less coronavirus means you get less sick – The Conversation
Masks slow the spread of SARS-CoV-2 by reducing how much infected people spray the virus into the environment around them when they cough or talk. Evidence from laboratory experiments, hospitals and whole countries show that masks work, and the Centers for Disease Control and Prevention recommends face coverings for the U.S. public. With all this evidence, mask wearing has become the norm in many places.
I am an infectious disease doctor and a professor of medicine at the University of California, San Francisco. As governments and workplaces began to recommend or mandate mask wearing, my colleagues and I noticed an interesting trend. In places where most people wore masks, those who did get infected seemed dramatically less likely to get severely ill compared to places with less mask-wearing.
It seems people get less sick if they wear a mask.
When you wear a mask – even a cloth mask – you typically are exposed to a lower dose of the coronavirus than if you didn’t. Both recent experiments in animal models using coronavirus and nearly a hundred years of viral research show that lower viral doses usually means less severe disease.
No mask is perfect, and wearing one might not prevent you from getting infected. But it might be the difference between a case of COVID-19 that sends you to the hospital and a case so mild you don’t even realize you’re infected.
Exposure dose determines severity of disease
When you breathe in a respiratory virus, it immediately begins hijacking any cells it lands near to turn them into virus production machines. The immune system tries to stop this process to halt the spread of the virus.
The amount of virus that you’re exposed to – called the viral inoculum, or dose – has a lot to do with how sick you get. If the exposure dose is very high, the immune response can become overwhelmed. Between the virus taking over huge numbers of cells and the immune system’s drastic efforts to contain the infection, a lot of damage is done to the body and a person can become very sick.
On the other hand, if the initial dose of the virus is small, the immune system is able to contain the virus with less drastic measures. If this happens, the person experiences fewer symptoms, if any.
Your Coronavirus Test Is Positive. Maybe It Shouldn’t Be. – New York Times
The usual diagnostic tests may simply be too sensitive and too slow to contain the spread of the virus.
Some of the nation’s leading public health experts are raising a new concern in the endless debate over coronavirus testing in the United States: The standard tests are diagnosing huge numbers of people who may be carrying relatively insignificant amounts of the virus.
Most of these people are not likely to be contagious, and identifying them may contribute to bottlenecks that prevent those who are contagious from being found in time. But researchers say the solution is not to test less, or to skip testing people without symptoms, as recently suggested by the Centers for Disease Control and Prevention.
Instead, new data underscore the need for more widespread use of rapid tests, even if they are less sensitive.
Teen and children hospitalizations, deaths from coronavirus increasing: report – The Hill
Coronavirus-related hospitalizations and deaths of children and teens are on the rise, according to data compiled by the American Academy of Pediatrics.
Although data indicate younger children are less likely to catch or transmit the virus, the May 21-Aug. 20 dataset shows a similar rise across states. Complicating matters is the fact that states use different grouping strategies, with many putting infants and teens in the same category, The New York Times notes.
Sean O’Leary, vice chairman of the American Academy of Pediatrics’s committee on infectious diseases, said that infections among children appear to increase with general community spread. He added that, as with adults, Black and Latino children appear to be at disproportionate risk of hospitalization.
“Anyone who has been on the front lines of this pandemic in a children’s hospital can tell you we’ve taken care of lots of kids that are very sick,” O’Leary told the Times. “Yes, it’s less severe in children than adults, but it’s not completely benign.”
With testing disrupted, storm-hit Louisiana watches other measures of the virus and sees trouble. – New York Times
Many dangers linger in Louisiana since Hurricane Laura, Gov. John Bel Edwards has warned: Downed power lines. Falling debris. Carbon monoxide poisoning from generators, the cause of more than half of storm-related deaths.
And the coronavirus. It has killed 400 times as many Louisianans as the storm, the governor noted, “just to put things in perspective, for whatever this may be worth.”
… Experts warned that the storm stood to worsen the coronavirus’s spread. Residents face more exposure while staying with relatives and friends or cleaning their property, or in other circumstances where it is difficult to maintain social distance. That may be especially true in the southwest, where hundreds of thousands of people lack power and may not see it return for days.
“If we think of Laura on top of Covid or Covid on top of Laura, it’s new and overwhelming,” Susanne Straif-Bourgeois, a professor at the L.S.U. Health Sciences School of Public Health who studies pandemics, told The New Orleans Advocate and Times-Picayune, which reported that the storm recovery provided fertile ground for new infections. “We’ve never had to deal with this before.”
New cases are rising by more than 5% in 26 states – CNBC
New cases of the coronavirus are rising by more than 5%, based on a seven-day average, in 26 states, according to a CNBC analysis of data compiled by Johns Hopkins University.
One week ago, new cases were rising by at least that much in just 12 states. While new cases are falling in former hot spots such as Arizona, California, Florida and Texas, according to CNBC’s analysis of Hopkins data, outbreaks are growing in a number of states, including Alabama, Iowa, Michigan, Missouri, North Carolina and the Dakotas.
The rise in new cases comes about two weeks after Director of the Centers for Disease Control and Prevention Dr. Robert Redfield said the middle of the country “is getting stuck” when it comes to combating the virus.
Cellphone location data could help predict COVID-19 trends, new research finds – CNN
Cell phone location data could be useful when it comes to predicting future trends in COVID-19 cases, according to new research published Monday in the journal JAMA Internal Medicine.
“Perhaps the most important observation of this study was that a decrease in activity at the workplace, transit stations, and retail locations and an increase in activity at the place of residence was associated with a significant decline in COVID-19 cases at 5, 10 and 15 days,” said the researchers, led by Dr. Shiv Sehra at Harvard Medical School.
For example, counties with the greatest use of cell phones in residential locations had a 19% lower growth rate of new cases at 15 days compared with those counties that had the lowest level of home usage.
The researchers also found that activity at grocery stores and areas that were classified as parks was not strongly associated with rates of growth in cases. However, assessing the direct effect of individual activities is difficult, they said.
The researchers used publicly available cell phone location data and new daily reported cases per capita in each US county to evaluate the association between cell phone activity on a given day, in a number of different locations, and the rate of growth in new COVID-19 cases five, 10 and 15 days later.
They found that there was a marked change in activities shortly before stay-at-home orders were issued in individual states, which included less activity in locations outside the home.
Urban counties with higher population levels and higher numbers of cases per capita had a greater increase in cell phone usage inside the home after stay-at-home orders, the researchers found.
193 passengers and crew ordered to self isolate after seven people on holiday flight contract coronavirus – Bioreports
At least seven passengers on a plane from Zante, Greece, to Cardiff, Wales, have tested positive for coronavirus after catching it from three infectious people on the flight.
All 193 passengers and crew on the TUI flight on August 25 have now been ordered self-isolate, according to a statement from Public Health Wales.
A passenger on the plane, Stephanie Whitfield, told the BBC the journey was a “debacle,” and that many of those on board had removed their masks. “The flight was full of selfish ‘covidiots,'” she added.
A TUI spokesperson said passenger health and safety “is always our priority” in an emailed statement sent to Bioreports. “We are concerned to hear of Mrs Whitfield’s claims,” it added.
“Our crew are trained to the highest standards and in line with European Union Aviation Safety Agency (EASA) guidelines. Passengers are informed prior to travel and via PA announcements on the flight that they have to wear masks throughout and are not allowed to move around the cabin,” reads the statement.
“Masks can only be removed when consuming food and drink,” the TUI spokesperson said. “A full investigation is now underway as these concerns weren’t reported during the flight.”
The following are foreign headlines with hyperlinks to the posts
Paris to make free COVID tests available in the capital
Spitting at politicians infringes constitution, German minister says
India Is Becoming the World’s New Virus Epicenter
Amazon tribal chief diagnosed with coronavirus
The virus is resurging in Spain, which reported 53,000 new cases in the past week.
India now has the third-highest death toll from the virus.
Canada to purchase 76 million doses of Novavax vaccine
WHO warns that ‘no country can just pretend the pandemic is over’
The following are additional national and state headlines with hyperlinks to the posts
Once a COVID-19 epicenter, Arizona emerges from lockdown
Man arrested in connection to shooting over social distancing rules at Wawa in Juniata [Philadelphia]
Lawmakers press CDC for guidance on celebrating Halloween during pandemic
New Jersey governor allowing limited indoor dining
Dozens of inmates at West Virginia prison test positive for coronavirus
In-Person Voting ‘Low Risk Activity,’ No ‘Detectable Surge’ in Wisconsin
Woman Kicked Out of Bingo Hall for Refusing to Wear a Mask
Philadelphia Mayor Under Fire for Dining Inside During Ban in Home City
New Jersey will allow for movie theaters to reopen and indoor dining to resume on Friday.
Dozens of students suspended as coronavirus outbreak emerges at New York college, chancellor says
Are drinking bans helping to stop the spread of Covid-19?
Today’s Posts On Econintersect Showing Impact Of The Pandemic With Hyperlinks
August 2020 Texas Manufacturing Marginally Declined But Still In Expansion
What Is The Impact Of School Closures During The Pandemic?
Explaining The Puzzling Behavior Of Short-Term Money Market Rates
Coronavirus INTERACTIVE Charts
include($_SERVER[‘DOCUMENT_ROOT’].’/pages/coronavirus.htm’); ?>
Analyst Opinion of Coronavirus Data
There are several takeaways that need to be understood when viewing coronavirus statistical data:
- The global counts are suspect for a variety of reasons including political. Even the U.S. count has issues as it is possible that as much as half the population has had coronavirus and was asymptomatic. It would be a far better metric using a random sampling of the population weekly. In short, we do not understand the size of the error in the tracking numbers.
- Just because some of the methodology used in aggregating the data in the U.S. is flawed – as long as the flaw is uniformly applied – you establish a baseline. This is why it is dangerous to compare two countries as they likely use different methodologies to determine who has (and who died) from coronavirus.
- COVID-19 and the flu are different but can have similar symptoms. For sure, COVID-19 so far is much more deadly than the flu. [click here to compare symptoms]
- From an industrial engineering point of view, one can argue that it is best to flatten the curve only to the point that the health care system is barely able to cope. This solution only works if-and-only-if one can catch this coronavirus once and develops immunity. In the case of COVID-19, herd immunity may need to be in the 80% to 85% range. WHO warns that few have developed antibodies to COVID-19. At this point, herd immunity does not look like an option although there is now a discussion of whether T-Cells play a part in immunity [which means one might have immunity without antibodies]
- Older population countries will have a higher death rate.
- There are at least 8 strains of the coronavirus. New York may have a deadlier strain imported from Europe, compared to less deadly viruses elsewhere in the United States.
- Each publication uses different cutoff times for its coronavirus statistics. Our data uses 11:00 am London time. Also, there is an unexplained variation in the total numbers both globally and in the U.S.
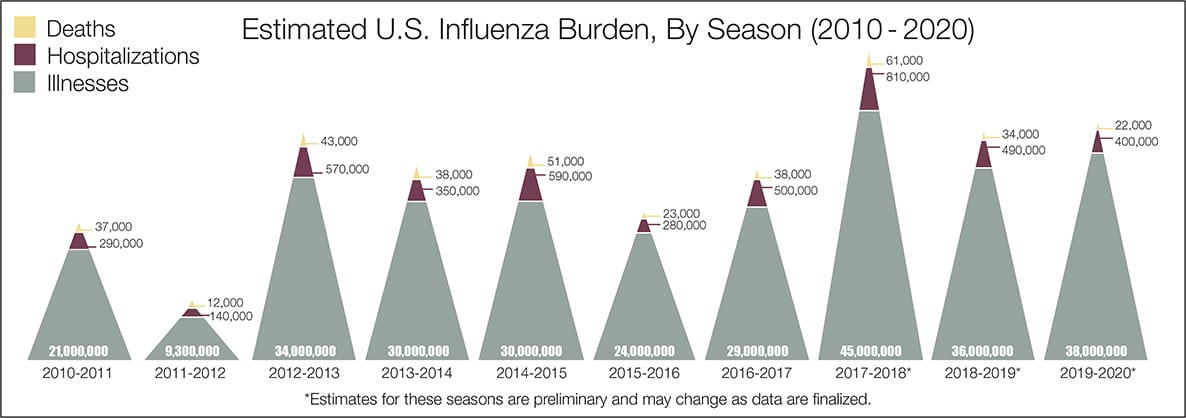
- The real question remains if the U.S. is over-reacting to this virus. The following graphic from the CDC puts the annual flu burden in perspective [click on image to enlarge]. Note that using this data is dangerous as the actual flu cases are estimated and not counted – nobody knows how accurate these guesses are.
What we do not know about the coronavirus [actually there is little scientifically proven information]. Most of our knowledge is anecdotal, from studies with limited subjects, or from studies without peer review.
- How many people have been infected as many do not show symptoms?
- Masks do work.
- Do we develop lasting immunity to the coronavirus? Another coronavirus – the simple cold – does not develop long term immunity.
- To what degree do people who never develop symptoms contribute to transmission?
- The US has scaled up coronavirus testing – and the accuracy of the tests has been improving. However, if one loses immunity – the coronavirus testing value is reduced.
- Can children widely spread coronavirus? [current thinking is that they are becoming a major source of the pandemic spread]
- Why have some places avoided big coronavirus outbreaks – and others hit hard?
- What effect will the weather have? At this point, it does not seem hot weather slows this coronavirus down – and it seems air conditioning contributes to its spread.
- Outdoor activities seem to be a lower risk than indoor activities.
- Can the world really push out an effective vaccine in 12 to 18 months?
- Will other medical treatments for Covid-19 ease symptoms and reduce deaths? So far only one drug (remdesivir) is approved for treatment.
- A current scientific understanding of the way the coronavirus works can be found [here].
Heavy breakouts of coronavirus have hit farm workers. Farmworkers are essential to the food supply. They cannot shelter at home. Consider:
- they have high rates of the respiratory disease [occupational hazard]
- they travel on crowded buses chartered by their employers
- few have health insurance
- they cannot social distance and live two to four to a room – and they eat together
- some reports say half are undocumented
- they are low paid and cannot afford not to work – so they will go to work sick
- they do not have access to sanitation when working
- a coronavirus outbreak among farmworkers can potentially shutter entire farm
The bottom line is that COVID-19 so far has been shown to be much more deadly than the data on the flu. Using CDC data, the flu has a mortality rate between 0.06 % and 0.11 % Vs. the coronavirus which to date has a mortality rate of 4 % [the 4% is the average of overall statistics – however in the last few months it has been hovering around 1.0%] – which makes it between 10 and 80 times more deadly. The reason for ranges:
Because influenza surveillance does not capture all cases of flu that occur in the U.S., CDC provides these estimated ranges to better reflect the larger burden of influenza.
There will be a commission set up after this pandemic ends to find fault [it is easy to find fault when a once-in-a-lifetime event occurs] and to produce recommendations for the next time a pandemic happens. Those that hate President Trump will conclude the virus is his fault.
Resources:
- Get the latest public health information from CDC: https://www.coronavirus.gov .
- Get the latest research from NIH: https://www.nih.gov/coronavirus.
- Find NCBI SARS-CoV-2 literature, sequence, and clinical content: https://www.ncbi.nlm.nih.gov/sars-cov-2/.
- List of studies: https://icite.od.nih.gov/covid19/search/#search:searchId=5ee124ed70bb967c49672dad
include(“/home/aleta/public_html/files/ad_openx.htm”); ?>